Ebony Foreman-Broaddus knows she is fortunate. She and her husband served with the Marines in Iraq before they married. They now enjoy a comfortable life in Conyers, Georgia, where they are raising two sons, ages 8 and 6, and a daughter, age 1. All are healthy and were born full term.
Broaddus is well aware that other African American women often experience adverse birth outcomes. Women in her racial group have a 1.5 times higher risk of preterm birth than Caucasian women, a statistic that makes preterm birth the leading cause of infant mortality in the African American population. While pregnant with her daughter, Broaddus enrolled in a School of Nursing study examining the underlying causes of preterm birth among some 500 pregnant African American women in metro Atlanta. The study, and research in general, are important to her.
“If I can help somebody figure out why preterm births and infant deaths occur, I’m all for it,” says Broaddus. “My sister passed away from SIDS [sudden infant death syndrome] when she was a few months old, so I want to do anything I can to help. I know a lot of African American women who have this notion that they don’t need to participate in research. When things happen to them they will say, ‘why wasn’t I told about this or why didn’t I know about this?’ We all need to expand our mindset and open our eyes to learn why certain things happen to us and our children.”
Specifically, Broaddus is helping researchers understand how biobehavioral determinants—the biological, social, behavioral, and environmental factors of health—influence the microbiome of African American women during pregnancy and whether disruption of the microbiome—the trillions of microbes that populate the body—may cause preterm birth.
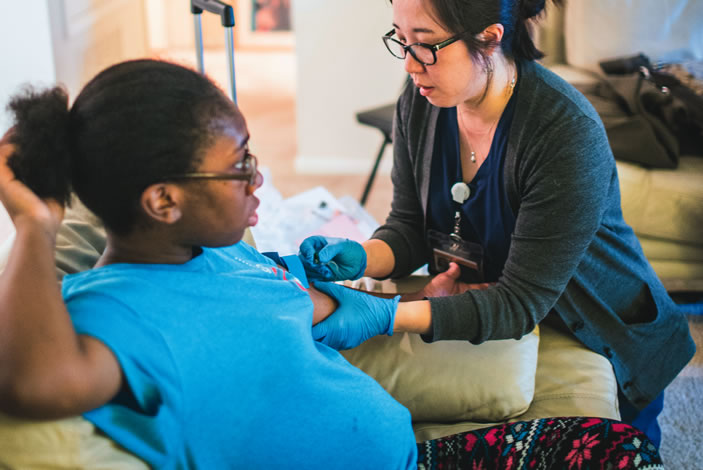
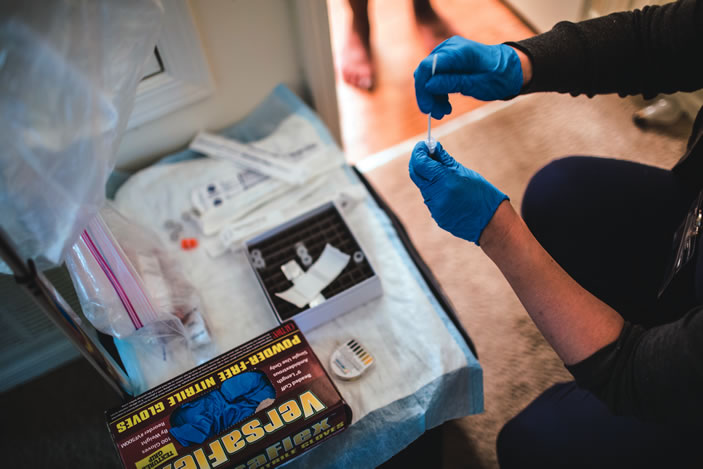
To date, nearly 300 expectant mothers ages 18 to 35 have enrolled in the longitudinal study, led by nursing researchers Elizabeth Corwin PhD RN FAAN and Anne Dunlop MD MPH and funded by the National Institute of Nursing Research. Participants agree to provide biological samples—via oral, vaginal, and rectal swabs and blood draws—during two prenatal clinic visits (at eight to 14 weeks and 24 to 30 weeks of pregnancy) at Grady Memorial Hospital or Emory University Hospital Midtown. Data also are collected from their medical records after their babies are born.
Researchers are analyzing the women’s samples in Emory laboratories to characterize the structure and dynamics of the vaginal, oral, and gut microbiome in order to determine which microbiome patterns may be linked to preterm birth. And they are identifying how biobehavioral determinants affect each microbiome during pregnancy.
Launched in 2014, the maternal microbiome project has yielded preliminary data for more than 250 women, with microbiome analysis completed for 50 women. To date, there has been a study retention rate of nearly 90 percent during pregnancy and a preterm birth rate of 15 percent. At least half of these women have experienced childhood trauma, such as family disruption, emotional or sexual abuse, and neglect. Income levels range from low to high.
“We’re learning that this is a very high-risk group of women,” says Corwin of the cohort.
The maternal microbiome study led by Corwin and Dunlop will yield results in other ways. It forms one pillar of a new children’s environmental health center involving four Emory University units—the School of Nursing, Rollins School of Public Health, the School of Medicine and Emory College of Arts and Sciences.
Formed last fall, the Center for Children’s Health, the Environment, the Microbiome, and Metabolomics (C-CHEM2) is gearing up to study factors affecting the environment of fetus and child and their impact on birth outcomes and the microbiome and neurodevelopment of infants.
One of 15 children’s environmental health centers in the nation and the only one in the Southeast, C-CHEM2 is the first such center to be based in a nursing school and to focus on the microbiome. Funding support comes from the National Institute of Environmental Health Sciences.
When the federal agency issued a call for proposals to study children’s environmental health with an emphasis on disparities, Linda McCauley, dean of the School of Nursing, and Barry Ryan PhD MS, professor of environmental health at Rollins, began talking. Both are experts in conducting community-based research on exposures to environmental toxicants and serve as dual principal investigators for C-CHEM2.
“Dr. Ryan pulled a lot of people together to talk about submitting a proposal, and it soon became clear that we were the program with a pillar study already in place,” Corwin explains. “We had a cohort of pregnant African American women who had delivered or were about to deliver and a pending follow-up study of their infants that fit the children’s health center concept well. From that point on, everything came together and the C-CHEM2 team was formed.”
“Health disparities start prenatally or even preconceptually,” adds Dunlop, who is using the same cohort to study the epigenetics of preterm birth with School of Medicine colleague Alicia Smith PhD. “It’s critical to initiate the investigation of the factors shaping child health disparities in the womb as early as possible during pregnancy.”