Low doses of the anti-cancer drug imatinib can spur the bone marrow to produce more innate immune cells to fight against bacterial infections, Emory and Winship Cancer Institute researchers have found.
The results were published this week in the journal PLOS Pathogens.
The findings suggest imatinib, known commercially as Gleevec, or related drugs could help doctors treat a wide variety of infections, including those that are resistant to antibiotics, or in patients who have weakened immune systems. The research was performed in mice and on human bone marrow cells in vitro, but provides information on how to dose imatinib for new clinical applications.
"We think that low doses of imatinib are mimicking 'emergency hematopoiesis,' a normal early response to infection," says senior author Daniel Kalman, PhD, associate professor of pathology and laboratory medicine at Emory University School of Medicine.
Imatinib, is an example of a "targeted therapy" against certain types of cancer. It,blocks tyrosine kinase enzymes, which are dysregulated in cancers such as chronic myelogenous leukemia and gastrointestinal stromal tumors.
Imatinib also inhibits normal forms of these enzymes that are found in healthy cells. Several pathogens – both bacteria and viruses – exploit these enzymes as they transit into, through, or out of human cells. Researchers have previously found that imatinib or related drugs can inhibit infection of cells by pathogens that are very different from each other, including tuberculosis bacteria and Ebola virus.
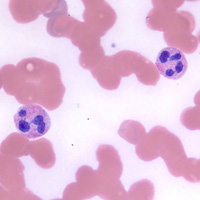
In the new PLOS Pathogens paper, investigators show that imatinib can push the immune system to combat a variety of bacteria, even those that do not exploit Abl enzymes. The drug does so by stimulating the bone marrow to make more neutrophils and macrophages, immune cells that are important for resisting bacterial infection.
"This was surprising because there are reports that imatinib can be immunosuppressive in some patients," Kalman says. "Our data suggest that at sub-clinical doses, imatinib can stimulate bone marrow stem cells to produce several types of myeloid cells, such as neutrophils and macrophages, and trigger their exodus from the bone marrow. However, higher doses appear to inhibit this process."
The authors note that imatinib appears to stimulate several types of white blood cells, which may provide a limit on inflammation, rather than increasing neutrophils only, which can be harmful. The authors go on to suggest that imatinib or related drugs may be useful in treating a variety of infections in patients whose immune system is compromised, such as those receiving chemotherapy for cancer.
Co-first authors of the paper are former graduate students Ruth Napier (Microbiology and Molecular Genetics program) and Brian Norris (Immunology and Molecular Pathogenesis program). Collaborators included Edmund Waller, MD, PhD, professor of hematology and medical oncology at Emory University School of Medicine and director of the bone marrow and stem cell transplant program at Winship Cancer Institute, as well as colleagues from Emory's Departments of Medicine, and Pediatrics and MD Anderson Cancer Center and Saint Louis University.
The research was supported by the National Institute for Allergy and Infectious Diseases (R01A107246201, R01AI05606701) and the National Heart Lung and Blood Institute (5P01HL08773), and by the Institute Merieux.
