Scientists have identified new drugs that target the Nox2 enzyme directly, instead of acting as antioxidants.
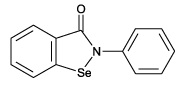
Nox enzymes are the main source of reactive oxygen species in cells. The structure of ebselen is shown here.
Scientists at Emory University School of Medicine have identified a new type of anti-inflammatory compound that may be useful in treating a wide range of conditions, including neurodegenerative and autoimmune diseases. These compounds inhibit the enzyme Nox2, part of a family of enzymes responsible for producing reactive oxygen species (ROS).
The results were published Thursday in the journal Chemistry & Biology.
“Nox2 inhibitors could be valuable with many conditions where inflammation plays a role,” says senior author David Lambeth, MD, PhD, professor of pathology and laboratory medicine at Emory University School of Medicine.
ROS and the Nox enzymes play vital roles in the immune and cardiovascular systems, but too much ROS leads to oxidative stress, linked with tissue damage and conditions such as stroke, heart failure and neurodegenerative diseases.
Antioxidants are supposed to absorb ROS such as peroxide and superoxide. However, many clinical studies examining antioxidants’ benefits have been disappointing. Compounds that inhibit the Nox enzymes would stop ROS production at the source, rather than mop them up like antioxidants do.
“We are taking a completely different approach,” says first author Susan Smith, PhD, Emory research assistant professor of pathology and laboratory medicine. “If a burst pipe is gushing water all over the basement, the first thing you need is a wrench to stop the water from flowing, instead of a mop.”
The Nox inhibitors that were already available to researchers are not specific enough for one enzyme over another. Smith collaborated with research scientist Jaeki Min and colleagues at the Emory Chemical Biology Discovery Center and Emory Institute for Drug Development to screen for compounds that inhibit Nox2. In particular, they searched for compounds that interfere with assembly of the Nox2 enzyme rather than targeting the catalytic site.
The screen for compounds that inhibit Nox2 led to the identification of ebselen, a drug that has been tested previously in clinical trials in acute stroke and more recently, hearing loss. Previous researchers had thought that ebselen acted by another mechanism. Smith and Lambeth say their results do not conflict with earlier reports, and ebselen may have several modes of action depending on the concentration. Ebselen inhibited the Nox2 enzyme and to a lesser extent, Nox1, but not other Nox enzymes.
A side effect of Nox2 inhibition could be impairment of immune responses to bacteria and fungi, Lambeth says. One of Nox2’s main functions in immune cells is to produce a toxic burst of ROS for killing bacteria and fungi.
People with an inherited deficiency in Nox2 develop chronic granulomatous disease (CGD), and are unable to fight off common infections. However, short-term or incomplete inhibition could have therapeutic effects without disabling antibacterial activity. CGD carriers who have reduced but residual Nox2 activity do not display symptoms.
Lambeth says the identification of ebselen is a starting point for refining drugs that target Nox2 and other Nox enzymes.
“This is just the tip of the iceberg,” he says. “It’s a good sign that ebselen is relatively non-toxic. Through medicinal chemistry, it should be possible to generate even more potent inhibitors, which could be candidates for drug development.”
The research was supported by the National Institute of Mental Health (R03 MH083234) and the National Cancer Institute (CA084138 and R01CA084138-08S1).
Reference: S.M.E. Smith et al Ebselen and congeners inhibit NADPH oxidase-2 dependent superoxide generation by interrupting the binding of regulatory subunits. Chem. Bio. 19, 752-763 (2012).
