Long Road Home
Emory Healthcare Veterans Program marks five years of helping heal the invisible wounds of military service

The numbers are staggering. More than 5 million post-9/11 service veterans have transitioned from the military back to civilian life, an average of 200,000 veterans each year. The transition isn't always easy.

Candace Baker woke up the morning of January 1, 2018, and said to herself: Something’s got to give.
Medically retired from the Army since 2011, Baker was spiraling downward. Chronic pain, post-surgery complications and post-traumatic stress disorder (PTSD) had eroded her ability to navigate the daily demands of work and life. The more time passed, the worse her situation became. For a time, she was “houseless,” as she calls it. Her only major possession was her car, and even that wasn’t in her name.
“I didn’t know who I was after I left the military,” says Baker, now 38. “The Army was all I’d ever wanted to do. It was my dream job. I needed something that would force me to deal with everything I’d lived through. When I heard about the Emory program and how intense it was, I said, ‘That’s it. That’s what I need.’”
Shortly thereafter, Baker sought care through the Emory Healthcare Veterans Program (EHVP) at the Emory Brain Health Center. In the two weeks of intensive outpatient treatment that followed, she began to write a new chapter for her life. “Mental health and physical health are inseparable,” she says. “It’s like peeling back an onion.”
Now marking its fifth anniversary, the Emory program has served more than 2,300 post-9/11 veterans and service members suffering from PTSD, traumatic brain injury, military sexual trauma, depression and anxiety.
During the early weeks of the COVID-19 pandemic, it expanded to include a remote intensive outpatient program. Adding telemedicine services allows Emory to work with even more veterans across the country. This new option delivers care in the comfort and privacy of the warrior’s home — and early results have been comparable to the established face-to-face program.
Emory’s program is part of the Warrior Care Network, a national initiative funded by the Wounded Warrior Project that works to meet the needs of thousands of post–9/11 veterans, regardless of their ability to pay.
“It’s an honor to be one of only four academic medical centers in the U.S. supported by the Wounded Warrior Project’s Warrior Care Network,” says Emory President Gregory L. Fenves. “The entire Emory team considers it a privilege to serve our veterans and their families.”
According to a survey published in the American Journal of Preventive Medicine, health remained the top concern for veterans both at three months and six months following their return home. Of survey respondents, 53% reported a chronic health condition, 33% reported a mental health condition and approximately 40% reported a chronic pain condition. The report concluded there is a need for “bolstered support” to prevent the development of “chronic readjustment challenges” in the veteran population.
Emory Healthcare providers, researchers and educators are helping to create a healthier long-term future for veterans. Across the Woodruff Health Sciences Center, faculty are pioneering holistic and increasingly personalized treatments. And they are strengthening alliances with the Atlanta VA Health Care System and other partners.

Join the Emory community as we recognize Veterans Day 2020.
The virtual program will open with a recorded ceremony on Emory’s Quadrangle honoring veterans. A live panel discussion will follow, with Emory alumni service members exploring what it means to lead through crisis, especially in 2020.
Panelists include Carlissa Carson 08L, Jon Keen 11MBA, Raye Perez 20MBA and Felicia Warren 99Ox 01C 08PH.
Emory President Gregory L. Fenves will deliver opening remarks. Jeffrey Rosensweig, Goizueta Business School associate professor of finance and founding faculty sponsor for the Emory Veterans Association, will moderate the discussion.
Watch live on Emory University’s Facebook page.
As many as 20% of Iraq and Afghanistan war veterans suffer from PTSD, according to the Veterans Affairs Department.


Navy Veteran Trent Burgess with his daughter, who "has her dad back" after his work to overcome his PTSD.
Navy Veteran Trent Burgess with his daughter, who "has her dad back" after his work to overcome his PTSD.
Trent Burgess was on deployment with the Naval Civil Engineer Corps in Iraq when he witnessed a child’s violent death in the middle of a crowded city street. He was 21 at the time and what he saw unmoored him. He didn’t talk about it afterward. That was the culture of the Navy, he says.
“I never talked about it, my unit never talked about it, the guys who watched it happen never talked about it,” he says. Returning home, he went 12 years without talking about it. He tried to resume a normal life but couldn’t find his footing. By 2018, PTSD had him at a breaking point.
“I was having trouble at work, in my marriage,” he says. “I was isolating myself. I ended up divorced. That was a real eye-opener.” He tried to treat his symptoms on his own, but nothing worked. Finally, Burgess called Emory. That call, he says, changed everything.
“PTSD is a disorder of avoidance,” says Barbara Rothbaum, professor of psychiatry, Paul A. Janssen Chair in Neuropsychopharmacology and director of the Emory Healthcare Veterans Program. “Traditional treatments for veterans with PTSD have a dropout rate of around half. Our program has a 90% completion rate.”
What’s more, veterans are maintaining the gains they made even after they leave the program. Approximately 88% of veterans who participate in the program’s two-week Intensive Outpatient Program (IOP) say they have maintained their gains a full year after they graduate. And the 12% who did not maintain their gains say they still are better off than they were prior to enrolling.
“Veterans are learning how to apply the tools we taught them,” Rothbaum says. “They are building back their lives over time.”
Burgess went through the IOP for PTSD (the program has since expanded to offer an additional track for veterans with traumatic brain injury and one for substance use disorder). He remembers with gratitude the veterans and active service members he met and bonded with during those weeks and has stayed in contact with several of them.
Another highlight, he says, were the in vivo sessions, a form of prolonged exposure therapy where veterans are introduced to environmental stressors they otherwise might avoid.
“I don’t like having my back to the door,” he says. “And the first thing they did, they had us sit with our backs to the door. So I had to get used to that. I also don’t like crowds. So we went to Walmart. And I had to learn — okay, crowded, yes; bad situation, no. I had to train myself to see that there’s a difference.”

Navy Veteran Trent Burgess with his daughter, who "has her dad back" after his work to overcome his PTSD.
Now, a year-and-a-half later, Burgess has regained stability and recovered his confidence, though he says he’s still a work in progress. He works at a construction supply company in Alpharetta and is a proud father to an eighth-grade daughter.
“I’m back to being the person I wanted to be,” he says. “My daughter can especially tell the difference. She’s got her dad back.”
The health care needs of this growing veteran population, especially for those with PTSD and another common wartime condition, traumatic brain injury (TBI), continue long after their first year back on home soil.

For Candace Baker, asking for help after her medical discharge from the Army proved difficult.
Not only did she face bureaucratic challenges to getting the care and social services she needed, she confronted an even more insidious obstacle: her own inner critic.
“In the military,” she says, “everyone tries not to be the weakest link. Being able to hold your own — that’s everything.” When her physical condition first began to affect her ability to perform her Army duties — she was an Avenger Systems Repairer at the time — Baker ignored the warning signs and pushed through the pain. Her physical health deteriorated. Her emotional health suffered also.
The downward spiral finally ended when Baker reached out to Emory.

Army veteran Candace Baker experienced chronic pain and PTSD, but tried to tough it out before getting help at Emory.
Too many veterans drop out of treatment for PTSD and other chronic conditions because accessing care over time can pose a logistical challenge. Sheila Rauch, the Mark and Barbara Klein Distinguished Professor in Psychiatry and the deputy director of the Emory Healthcare Veterans Program, is tackling the accessibility question at Emory and at the Atlanta VA Medical Center, where she is director of research and program evaluation for the VA’s mental health service line.
“The biggest barrier,” Rauch says, “is getting the treatments that work to veterans where they are.” To that end, she’s developing and testing telemedicine and primary care treatment models for PTSD, so veterans can receive the best evidence-based care without having to seek out a specialty mental health office.
The remote intensive outpatient program launched in response to COVID-19 “delivers life-transforming care in the comfort and privacy of the warrior’s home,” Rothbaum says. The option is available for warriors living in Georgia and other states where approval has been granted. “We are continuing to serve veterans, just teleworking. We are still conducting intakes. We are seeing outpatients via telemedicine.”

Professor of Psychiatry Barbara Rothbaum is executive director of the Emory Healthcare Veterans Program and a national leader in virtual reality therapy.
The social work and wellness team also compiled a library of online resources to help warriors practice mindfulness, develop listening skills, manage family stress and strengthen resilience. And veteran outreach coordinators set up virtual meet-ups to help warriors connect with each other in real time.
Follow-up care for veterans who do participate in intensive treatment programs remains key. Each Warrior Care Network site has a VA-based social worker on the team who helps veterans with continuity of care, even after they have returned to their regular health care provider.
For her part, Baker credits the Emory team with introducing her to additional veteran service organizations after she graduated from the program. She now volunteers with The Mission Continues in her Virginia hometown. When asked how she feels about the military today, she fights back tears.
“It’s a double-edged sword,” she says. “I will never love anything like I loved the idea of the military. Some days I think I will never love anything that much again. But I can’t go back. I have to move on.”
“We need to get the message out to veterans,” Rothbaum says. “You can take your life back."

Army veteran Candace Baker experienced chronic pain and PTSD, but tried to tough it out before getting help at Emory.
Army veteran Candace Baker experienced chronic pain and PTSD, but tried to tough it out before getting help at Emory.

Professor of Psychiatry Barbara Rothbaum is executive director of the Emory Healthcare Veterans Program and a national leader in virtual reality therapy.
Professor of Psychiatry Barbara Rothbaum is executive director of the Emory Healthcare Veterans Program and a national leader in virtual reality therapy.

Lieutenant General (ret.) William “Burke” Garrett III is executive adviser to the Emory Healthcare Veterans Program and uses outdoor and peer therapy, among other tools, to help veterans heal.
Lieutenant General (ret.) William “Burke” Garrett III is executive adviser to the Emory Healthcare Veterans Program and uses outdoor and peer therapy, among other tools, to help veterans heal.
Lieutenant General (ret.) William “Burke” Garrett III has made it his mission to help veterans reclaim their lives and health, partly through outdoor therapy.
As executive adviser to the Emory Healthcare Veterans Program, he brings nearly four decades of leadership experience to his role, which includes building new alliances and strengthening Emory’s existing relationships with the U.S. military, the Wounded Warrior Project and community and government partners.

Lieutenant General (ret.) William “Burke” Garrett III is executive adviser to the Emory Healthcare Veterans Program and uses outdoor and peer therapy, among other tools, to help veterans heal.
Garrett also brings his love of the North Georgia mountains. He received his military training at the University of North Georgia in Dahlonega and spent summers working with the Youth Conservation Corps in the Chattahoochee National Forest and on the Appalachian Trail. He makes a point of spending time outdoors with those enrolled in the Emory program, and has offered guided hikes at Kennesaw Mountain National Battlefield Park for veterans.

A group from Emory Healthcare Veterans Program on a pre-pandemic hike at Kennesaw Mountain, which helped provide both physical and emotional healing.
A group from Emory Healthcare Veterans Program on a pre-pandemic hike at Kennesaw Mountain, which helped provide both physical and emotional healing.
“A mountain is the perfect symbol of the challenges we face in life,” he says. “Every challenge we conquer serves to strengthen not only our will, but our confidence, and therefore our ability to overcome future obstacles.”
While the program’s focus remains on delivering care, the research driving this care forward has inspired Garrett. The future of veterans’ health, he says, lies in personalized treatment.
“We are excited about the potential of biomarkers to dramatically improve the precision of diagnostics and the ability to personalize treatments for veterans with PTSD,” he says.
Emory serves as the PTSD biomarker repository for the Warrior Care Network. The collection of blood and saliva samples from veterans who elect to participate is potentially game-changing. Data from this repository could help researchers predict who is more likely to experience PTSD. It could help with the development of treatment and prevention strategies.
It also could help identify which treatment will work best for any given veteran or service member, because there is no one-size-fits-all therapy when it comes to PTSD and its shattering effects.
The National Center for Veterans Analysis and Statistics estimated that nearly 700,000 veterans were living in Georgia in 2018.

Timothy Banik entered the U.S. Marine Corps when he was in high school. He was 18 and wanted to follow in his brother’s footsteps.
“I wasn’t ready for college,” he says. “I didn’t know what I wanted to do, but I knew I wanted to test myself. So I picked the Marine Corps, and I picked the infantry.”
He started boot camp in 2006 and served in the Marines for four years, including two overseas deployments in combat zones. He was emotionally unprepared to handle what he saw when he arrived at his first post in Fallujah, in Iraq’s Anbar Province.
“My first sight was of a destroyed city,” he says. “After that, I just wanted to make it home alive.”

Timothy Banik (second from left) poses with Iraqi children and fellow Marines during his military service. Photo courtesy of Banik.
By his second deployment, Banik wasn’t sure he would make it to his next birthday. He’d faced combat firsthand. He’d seen the bloody aftermath of improvised explosive devices (IEDs). Those sights would haunt him. “Maybe I’ll make it to 21 so I can get home and have my first legal drink,” he remembers thinking.
Discharged in 2010, Banik did take that first legal drink. Then he took another. He wound up relying on alcohol to self-medicate his symptoms of depression and PTSD.
He suffered from suicidal thoughts. He sought help but says the medication prescribed made him feel even worse. “I called the suicide hotline at the VA countless times,” he says. Not until his wife learned about the Emory program and urged him to enroll did he begin to chart a way forward.
Banik completed the intensive outpatient program in February 2018. The program taught him what he had experienced in war did not have to control or define him. He found the psychotherapy component of the program transformative.
“I had to believe that I deserved a better life,” he says. “That was hard at first.”
Today, at 32, Banik is a secondary market analyst at a bank. He and his wife recently bought a home. They have a dog, and they’re thinking about starting a family. Banik has started sharing his story with other veterans, connecting with Garrett and volunteering with him to lead a pre-pandemic hike up Kennesaw Mountain. Afterward, they took everyone out to breakfast and shared their stories.
“So many vets believe someone else deserves the help more,” Banik says. “I had to learn that if you think you need help, you deserve the help. End of story.”

Timothy Banik (second from left) poses with Iraqi children and fellow Marines during his military service. Photo courtesy of Banik.
Timothy Banik (second from left) poses with Iraqi children and fellow Marines during his military service. Photo courtesy of Banik.

Ursula Kelly, associate professor at the Nell Hodgson Woodruff School of Nursing and a nurse scientist at the Atlanta VA Health Care System, is pioneering research into the effects of yoga for PTSD.
Ursula Kelly, associate professor at the Nell Hodgson Woodruff School of Nursing and a nurse scientist at the Atlanta VA Health Care System, is pioneering research into the effects of yoga for PTSD.
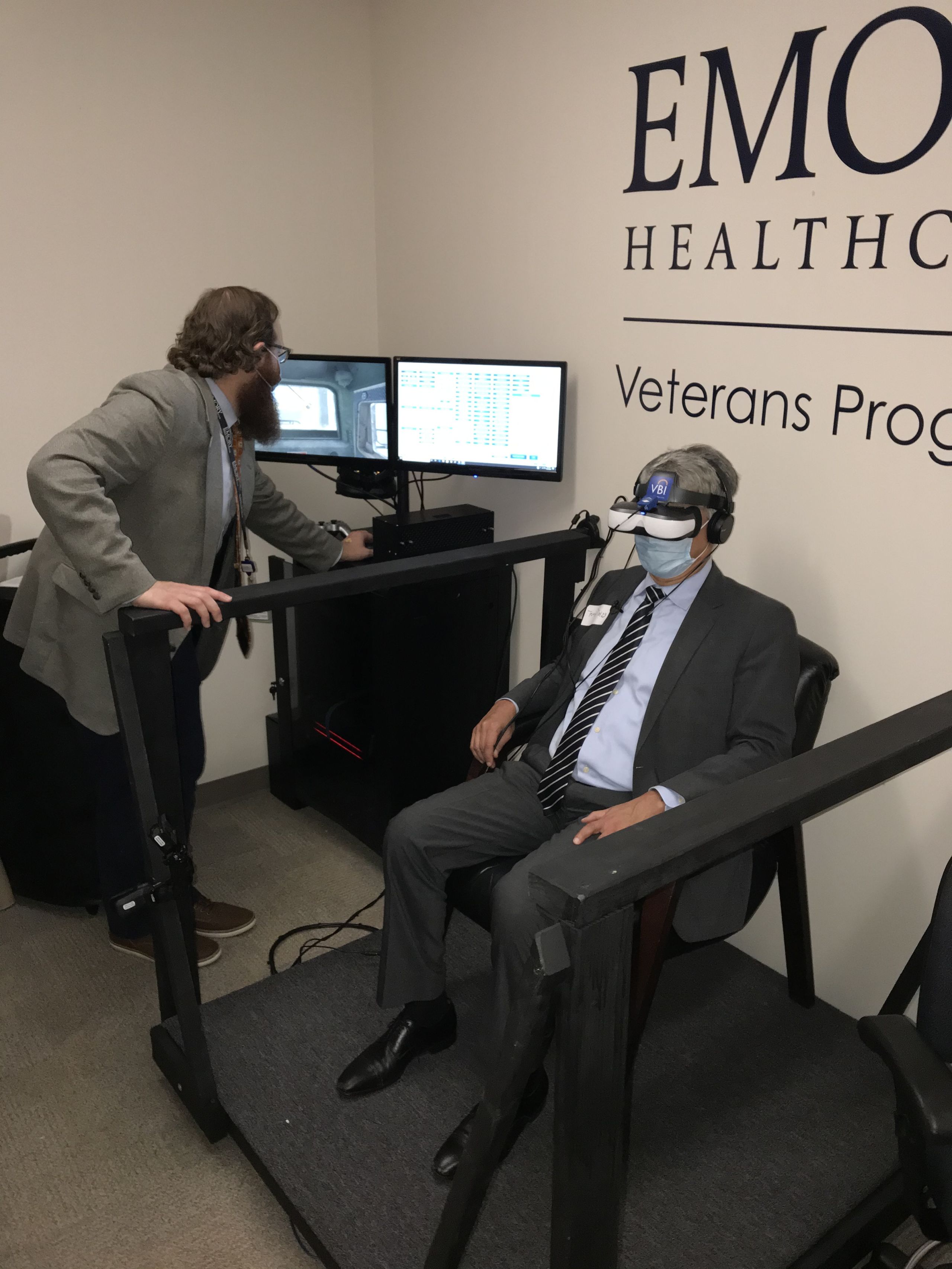
Virtual reality exposure therapy helps veterans and service members face their worst memories and move on with their lives. Here, Dr. Andrew Sherrill gives Emory President Gregory L. Fenves a demonstration of the technology as part of a recent tour of the program.
Virtual reality exposure therapy helps veterans and service members face their worst memories and move on with their lives. Here, Dr. Andrew Sherrill gives Emory President Gregory L. Fenves a demonstration of the technology as part of a recent tour of the program.
Listening to veterans means acknowledging that wounds of war do not come from combat alone, says Ursula Kelly, a nurse scientist at the Atlanta VA Health Care System.
Kelly is pioneering research into the effects of trauma-sensitive yoga for veterans who have experienced PTSD from combat or sexual trauma.
“There are differences between PTSD caused by combat and PTSD caused by sexual trauma,” she says. “Both are life-altering, but military sexual trauma often involves a deeply personal betrayal. These are the people — fellow service members and superiors — who were supposed to have your back. With PTSD related to military sexual trauma, not only are veterans dealing with the stigma of having PTSD, but there is the added stigma and victim-blaming associated with women’s sexual assault.”

Ursula Kelly, associate professor at the Nell Hodgson Woodruff School of Nursing and a nurse scientist at the Atlanta VA Health Care System, is pioneering research into the effects of yoga for PTSD.
The VA defines military sexual trauma as sexual assault or ongoing threatening sexual harassment while serving in the military. It is now so common the VA routinely asks all veterans if they have experienced it. Between 20% and 40% of female service members report having experienced military sexual trauma, depending on what study is being cited, according to Kelly. Male service members also experience military sexual trauma, but their reporting rates are much lower — 3% to 4% — though experts believe their actual rates are actually similar to women’s.
In research funded by the VA, Kelly and her colleagues are comparing the effectiveness of trauma-sensitive yoga to evidence-based psychotherapy for PTSD. She believes yoga, as an embodied treatment, offers an important tool for healing over the long term.
How does yoga help? The answer might seem counterintuitive, she says. Yoga works precisely because it does not require the patient to retell their story, at least not right away. Kelly’s theory is yoga has the opposite effect of PTSD on the nervous and immune systems — and provides a non-cognitive pathway to healing.
“For some survivors,” she says, “exposure therapy just isn’t possible right away. They’ve usually experienced multiple traumas throughout their lives. The complexity is just too great. ‘Telling your story’ is exceedingly difficult for these women.”
The results of her research to date are promising. Trauma-sensitive yoga is proving to be as effective as evidence-based psychotherapy (specifically, cognitive processing therapy) for treating PTSD and co-occurring depression in women with PTSD and military sexual trauma. Kelly isn’t looking to replace psychotherapy. But she thinks yoga could provide an alternative or serve as an additional treatment. Yoga helps people learn to regulate their emotions through their bodies, rather than through their thoughts and memories.
At the Emory Healthcare Veterans Program, yoga is offered to participants as a valuable general practice, though not as a specific treatment for PTSD.

Virtual reality therapy also is among the treatments offered to veterans in the program for a wide range of combat-related issues, including military sexual trauma-related PTSD. According to research conducted by Rothbaum’s team, virtual reality therapy holds promise for providing relief for veterans grappling with this particularly difficult set of experiences.
Rothbaum has long been a pioneer in virtual reality therapy for patients with phobias, anxiety, addictions or PTSD. Virtual reality exposure therapy involves having patients describe aloud their most traumatic memories while the therapist matches those descriptions using a computer-generated 3D environment.
“The virtual reality exposure system provides an effective treatment and allows for controlled delivery of sensory stimulation by the therapist,” she says.

Virtual reality exposure therapy helps veterans and service members face their worst memories and move on with their lives. Here, Dr. Andrew Sherrill gives Emory President Gregory L. Fenves a demonstration of the technology as part of a recent tour of the program.
Meanwhile, Kelly’s work at the VA serves as a reminder of how important skilled nurses and nurse scientists are for veterans’ health care nationwide.
Emory is one of 18 U.S. nursing schools competitively chosen by the Department of Veterans Affairs to participate in the VA Nursing Academic Partnership for undergraduate nursing students and graduate nurse practitioner students.
Since its launch at Emory in 2013, the VA Nursing Academic Partnership program has graduated more than 100 nursing students. More than 20 graduate nurse practitioner students have graduated since 2015, the start of the graduate arm of the program.
The program trains nurses to understand the unique and often chronic issues within the veteran population. Lisa Muirhead, associate professor of nursing at the Nell Hodgson Woodruff School of Nursing, serves as principal investigator for both programs.
“I’ve been most inspired by the willingness that veterans have shown to share their stories with our nursing students,” she says. “I’m also inspired by the growing interest in caring for veterans that our students express as they are immersed in the provision of veteran-centered care.”
There’s a lot that being in the military can and does prepare you for, says Banik, the Marine veteran:
“But they can’t teach you how to deal with the outcomes of war or what you might see in wartime situations. I want my fellow veterans to know that help is possible. Mental health is possible.
“Reaching into the deepest parts of your soul, that’s harder than battle. But it can be done,” Banik says.
By Stacia Pelletier. Leigh DeLozier contributed.
Contact the Veterans Program:
Any veteran who is interested can contact the Emory Healthcare Veterans Program at 888-514-5345 or online.

Emory has long supported veterans — changing lives not only through initiatives such as the Emory Healthcare Veterans Program, but also through programs that serve their educational and legal needs.
The Emory Veterans Association is a student-run group focused on providing support and opportunity for student veterans at Emory. EVA strives to make Emory a top destination for student veterans, offering networking, support and developmental opportunities for veterans and their families.
Through the Yellow Ribbon Program, degree-granting institutions of higher learning in the U.S. voluntarily enter into an agreement with the Veterans Administration to fund a portion of tuition expenses that exceed the annual VA tuition and fees benefit.
Undergraduate students planning military careers can participate in Army or Air Force ROTC through a cross-enrollment agreement with Georgia Tech. Students complete their undergraduate degrees at Emory and military training at Tech.

Emory is one of 18 nursing schools nationwide selected for the elite VA Nursing Academic Partnership (VANAP) program through the U.S. Department of Veterans Affairs. Undergraduate and graduate nursing students selected for the program gain valuable training in providing quality care for our nation’s veterans.
Launched in 2013, the Emory Law Volunteer Clinic for Veterans provides pro bono legal services for veterans, assisting them and their families with legal issues including disability claims before the Veterans Administration and subsequent appellate proceedings, estate work and discharge upgrades before the Department of Defense. Clinic representatives travel throughout the state to provide outreach, training and roughly 380 consultations annually.
Emory’s support for veterans on campus and in the community is enhanced by philanthropic support. Whether you are passionate about providing financial assistance for veterans who are students or growing the capacity of Emory to provide legal and health care services to veterans, your gift will benefit our nation’s heroes.

Learn more about Emory:
Emory University • Emory Woodruff Health Sciences Center • Emory News Center • Emory Health Digest

