COVID-19: Emory on the Front Lines
Emory Magazine | Spring/Summer 2020
Part 1 in a series of personal stories on how alumni, faculty and students are fighting the pandemic in a wide variety of ways.
AN ER DOCTOR'S PERSONAL SACRIFICES
Despite having to keep isolated from his family — including a newborn daughter — Emory emergency physician Justin Schrager soldiers on to treat COVID-19 patients and flatten the curve.
Justin Schrager 08PH 12M 15MR wants nothing more than to come home from work and scoop up his weeks-old baby girl into his arms. But as an emergency medicine physician at Emory University Hospital — where he’s exposed every day to patients who have been infected with the highly contagious COVID-19 coronavirus — Schrager knows the daddy-daughter cuddles and the tickling of her tiny little toes will have to wait.
Since health care workers on the front line run a high risk of contracting the virus, he has to take extraordinary precautions to avoid bringing it home and passing it along to his family. That means after a grueling overnight shift in the ER, Schrager can’t even come home and rest in his own bed. He has to isolate himself from those he loves, holing up alone in their garage apartment. So close, yet far away.

Dr. Justin Schrager 08PH 12M 15MR, Emergency Medicine Physician at Emory University Hospital, and Assistant Professor, Emory School of Medicine
He can’t even help his wife with changing diapers and the other non-stop demands of raising a newborn. Nor can Schrager help much in wrangling their other son and daughter — ages 4 and 6 — who now find themselves stuck at home since their schools have closed.
“We’re doing our best, though it’s just not the same as we had hoped this time to be,” Schrager says. “My wife was supposed to be recovering, spending quality time with the baby, the kids busy in school, me helping out, and everyone happy. Obviously, that’s not happening because of the coronavirus.”
They’re learning to make the best of it. On days off, when the weather’s nice, Schrager is able to spend time with his family sitting and chatting outside in the yard or going on walks together — all at a healthy distance, of course. Otherwise, phone calls, FaceTime, and Zoom meetings have become their primary ways to stay connected.
Luckily his wife, Rachel Patzer 07PH 11G — a renowned epidemiologist and associate professor in Emory’s School of Medicine — was better prepared than most for what needed to happen when COVID-19 came to the U.S.
“Both Rachel and I trained in epidemiology at the Rollins School of Public Health — where we met — and worked at the CDC,” Schrager says. “Then I went to Emory medical school, and Rachel completed her PhD. When the outbreak occurred in China and started moving from country to country, we tracked it and could read what direction it was going in the weeks before Rachel went into labor with our daughter. We understood the math behind the spread of the disease, and how communicable it was likely going to be.”
Together, shortly after their baby’s birth, the couple made the decision for Schrager to isolate himself from the rest of the family. “We surely weren’t the only people doing this before the sheltering-in-place declarations started,” he says. “Everyone working in emergency services and critical care — doctors, nurses, EMTs, support staff — knew early on they would have to make life-altering changes to their daily regimen to protect themselves and their families.”
But Patzer wanted to spread greater awareness about the sacrifices health care workers and their families around the globe were making. So she turned to Twitter.
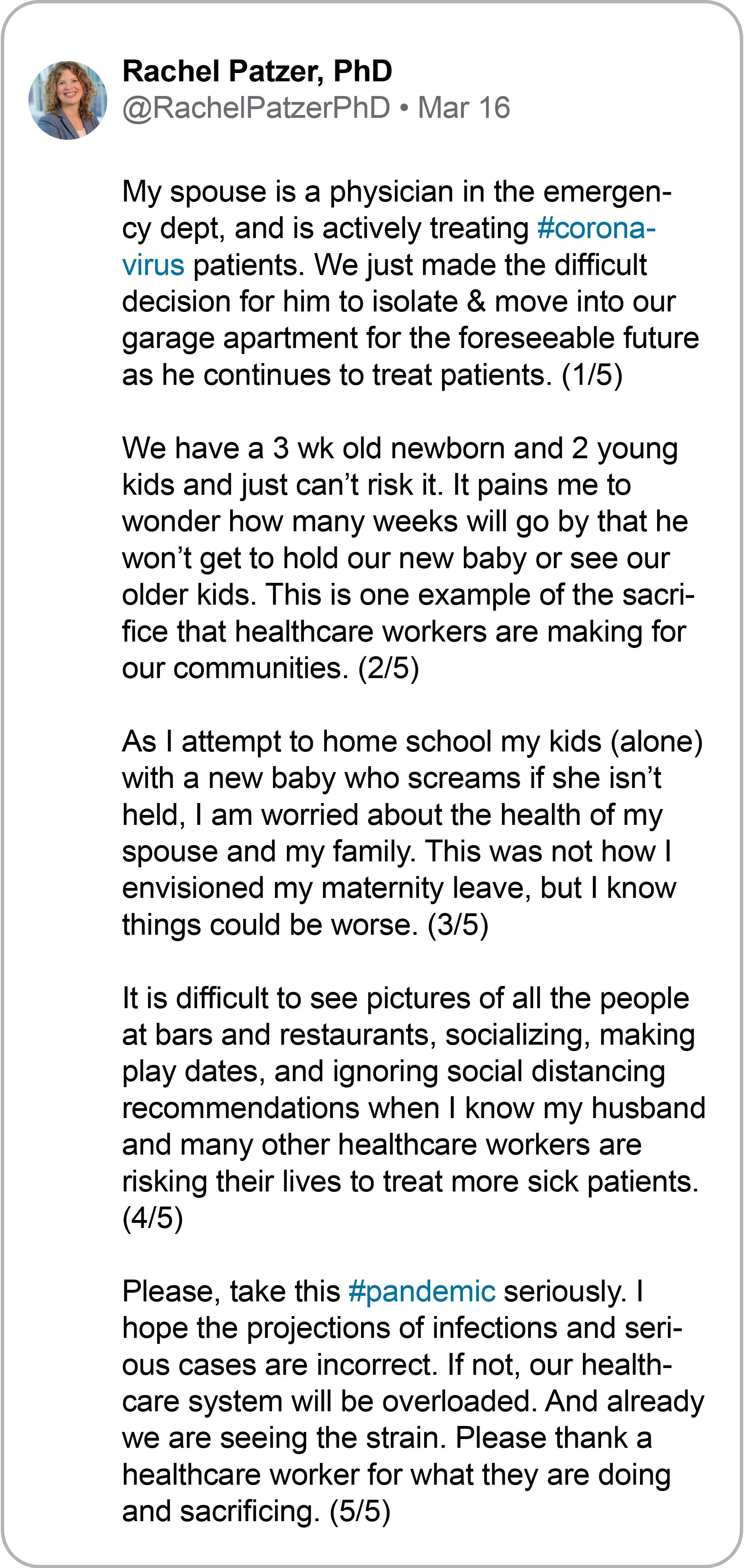
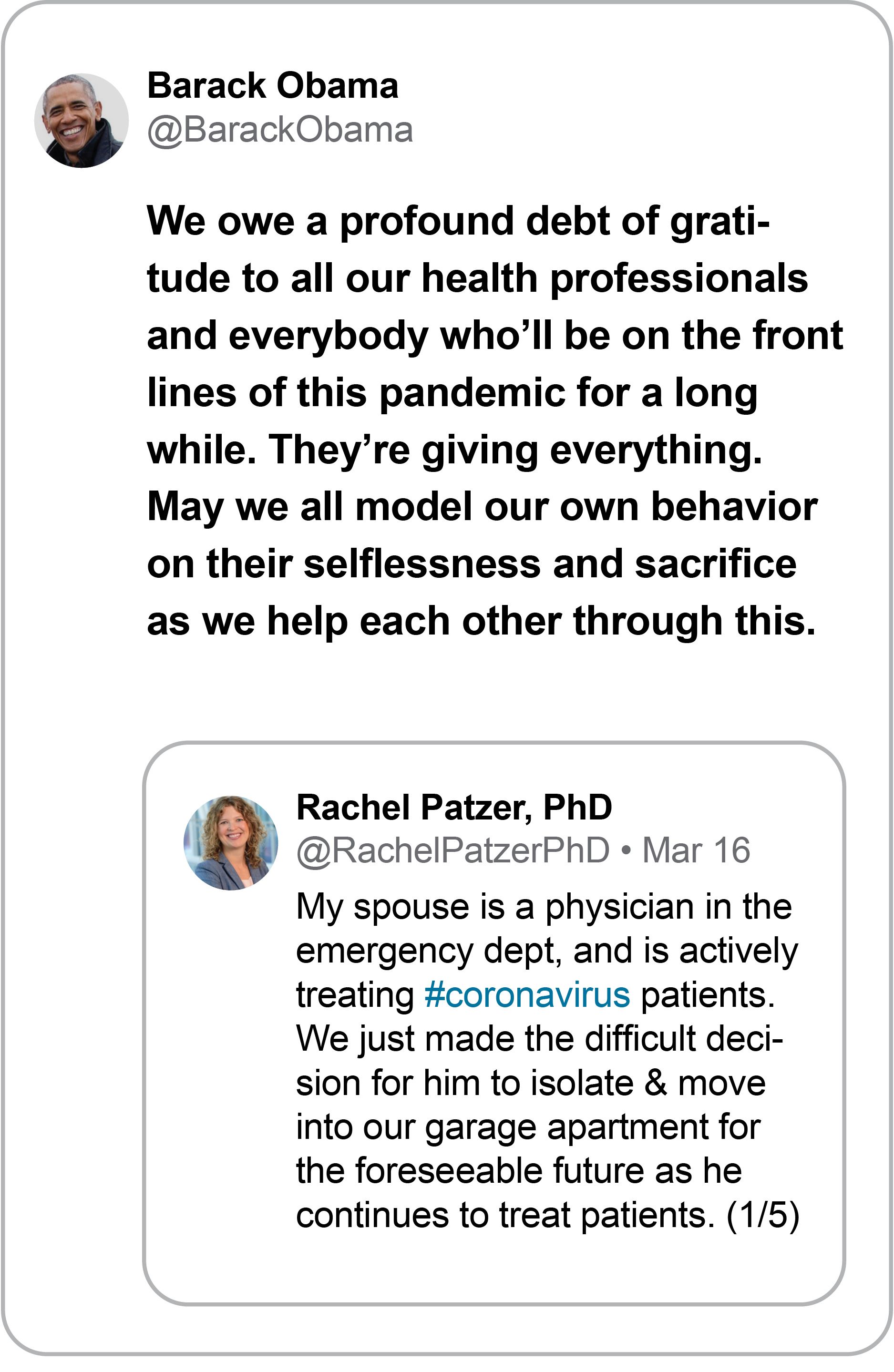
Her message quickly struck a nerve on the social platform, and tens of thousands of people responded to her thread. And then her message really went viral when former U.S. President Barack Obama retweeted it and added his own message of thanks to those on the front lines of COVID-19.

Dr. Justin Schrager 08PH 12M 15MR, Emergency Medicine Physician at Emory University Hospital, and Assistant Professor, Emory School of Medicine
Dr. Justin Schrager 08PH 12M 15MR, Emergency Medicine Physician at Emory University Hospital, and Assistant Professor, Emory School of Medicine
“THIS DISEASE REALLY SCARES ME”

Emory University Hospital Clifton Road
At Emory University Hospital, Schrager still treats numerous COVID-19 cases a day. He’s witnessed what the disease can do — and he’s afraid of it.
“I’ve been an ER doctor for a good while, trained at both Emory and Grady hospitals, so there’s not much I haven’t seen,” he says. “My fear threshold is pretty high, but this disease really scares me because it can cause people to become critically ill very quickly. Patients can come into the ER looking run down and coughing, like they have the common seasonal flu, and then in a matter of a few hours be unable to breathe, have to be intubated and put on a ventilator.”
Luckily, Emory is prepared better than most for outbreaks like the coronavirus. “Emory Healthcare, in particular, is blessed with national leaders in how to manage communicable disease outbreaks — evidenced by the successful response to Ebola more than five years ago — as well as how to treat patients and protect its health care workers,” Schrager says. “They’ve done literally everything I can think of to get us ready for pandemics like COVID-19.”
And while Schrager is backed by excellent intensive care and respiratory care teams, he knows that his counterparts around the U.S. are suffering. “Doctors are getting hit hard as patients flood the health care systems in a growing number of hot spots, and they’re running into shortages of resources and even ICU beds,” he says. “I don’t want to imagine what it would be like to ask for a ventilator for a patient and be told there wasn’t one available.”

Emory University Hospital Clifton Road
Emory University Hospital Clifton Road
FLATTENING THE CURVE
Another way to combat COVID-19 is to “flatten the curve” of infections, drawing them out over time — by having people practice social distancing and shelter at home — so hospitals and clinics aren’t flooded with patients all at once. Schrager has put himself in a unique position to help with the effort.
Last year, he co-founded software company Vital with his brother-in-law Aaron Patzer (founder of Mint.com) to help hospital emergency departments manage their workload and triage patients. With the outbreak of COVID-19, the duo foresaw an opportunity to help people self-triage and hopefully keep many of those with mild symptoms — and unchecked anxieties — at home and out of the ER.
“We diverted all of Vital’s resources to work with Emory University Healthcare to build an online tool called C19check.com,” Schrager says. “To be clear, it’s not a diagnostic tool — it won’t tell you if you have the coronavirus — but instead it allows people to check their symptoms and health risks to recommend what they should do next, according to CDC guidelines.”
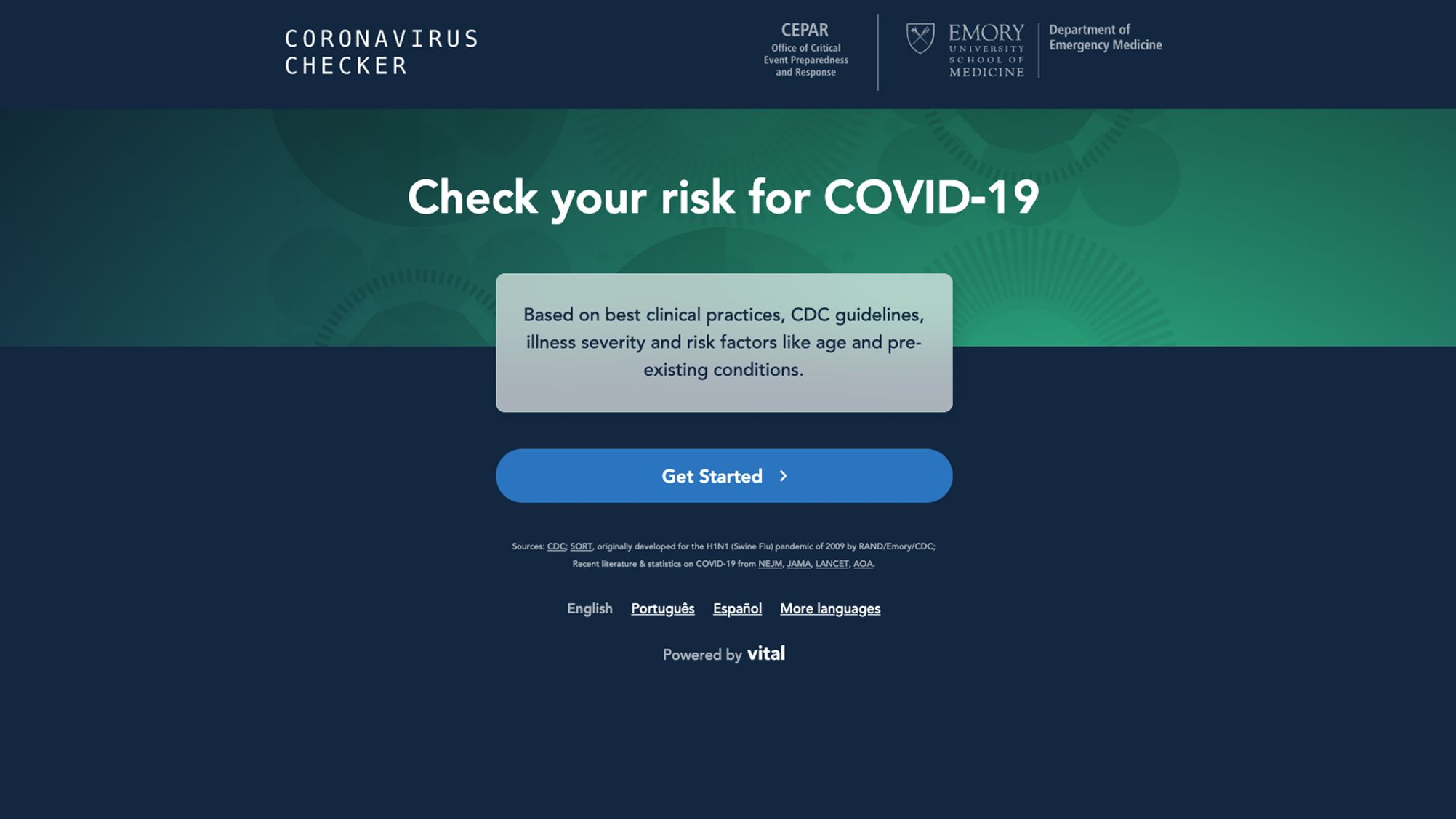
c19check.com
Based on the answers to questions about signs and symptoms, age and other medical problems, a person can use the free C19check.com tool to assess if they are high risk and need immediate medical attention, intermediate risk and should follow-up with their doctor, or low risk and should most likely administer self-care and recover at home.
Designed by the Vital team with guidance from the Emory Department of Emergency Medicine's Health DesignED Center and the Emory Office of Critical Event Preparedness and Response (CEPAR), the C19check.com website leverages the SORT algorithm first developed by Emory doctors more than a decade ago to manage and monitor the H1N1 virus pandemic.
“Doctors know that crowded waiting rooms could make the problem worse because people sick with COVID-19 could infect others, speeding the overall rate of infection,” says Dr. Alex Isakov, executive director of Emory’s CEPAR, and co-author of the SORT algorithm. “Keeping stress off the system and limiting exposure for at-risk populations is going to be key to managing the community spread of COVID-19.”
Developing C19check.com to help flatten the curve was also driven by a very selfish motive, Schrager admits.
“I promised my wife that while I’m unable to help take care of the kids and she’s having to manage everything on very little sleep, that I would spend my time in isolation to fight this epidemic in any way I could,” he says. “The sooner we can slow or halt the pandemic, the sooner I can get out of the garage and be with my family. When I’m not treating COVID-19 patients in the ER, I’m working on the site, as well as a few other coronavirus-related research projects.”
His main worry about the pandemic, moving forward, is the resiliency of the health care workforce. “It’s not a sprint — it’s a marathon,” Schrager says.
Story by Roger Slavens, design by Elizabeth Hautau, COVID-19 illustration by Satyen Tripathi.

c19check.com
c19check.com

Want to know more?
Please visit Emory Magazine, Emory News Center, Emory University and Emory COVID-19 Updates

