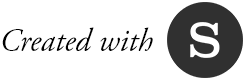The Learning Fields
Students care for Georgia's migrant farmworkers

Emory is home to two successful migrant health programs—one led by the Nell Hodgson Woodruff School of Nursing, the other by the Physician Assistant Program in the School of Medicine. Both can be life-changing for students and farmworkers alike.

Take Sharon Quinn 05N, who fell in love on a hot, humid day down in Moultrie, Georgia. But this was no summer romance. What began as a student learning experience in migrant health in 2005 has blossomed into a steadfast relationship that continues today.

Every June, Quinn makes the three-hour-plus drive from Atlanta to Moultrie in a van filled with donated supplies destined for a much-anticipated rendezvous with students and faculty from the Nell Hodgson Woodruff School of Nursing. Her van carries an assortment of goods—sheets, pillows, duvet covers, toiletries, bottled water, socks, flip flops, rubber boots, shirts, jeans, jackets, hats, and children’s goody bags—to share with migrant families in the area.
For the next two weeks, Emory student nurses—along with dental hygiene, physical therapy, and pharmacy students from six Georgia universities—will provide basic health care to workers who pick produce on farms surrounding Moultrie in the heart of Colquitt County. They also will visit farms in three neighboring counties.
Quinn proudly shows off the supplies she has stored in a room at Cox Elementary, where the workers’ children attend a special summer school. Nearby, boys and girls play in the school gym, where undergraduate and graduate student nurses do their annual health screenings.
Collecting, transporting, and distributing the supplies is a lot of work, Quinn admits. But she is in her happy place, nearly 200 miles away from her daily routine with Emory Healthcare in Atlanta.

Nursing faculty Erin Ferranti, Lori Modly, Judith Wold, and alumna Sharon Quinn take a respite during a night camp at Lewis Taylor Farms.
Nursing faculty Erin Ferranti, Lori Modly, Judith Wold, and alumna Sharon Quinn take a respite during a night camp at Lewis Taylor Farms.
“I came down here as a student and fell in love with the migrant health project,” she says. “Judy can’t get rid of me.”
Quinn is referring to Judith Wold 81MN, the Emory nursing professor who leads the annual Farmworker Family Health Program (FWFHP) in Moultrie. Now in its 25th year, the program is based in the Lillian Carter Center for Global Health & Social Responsibility, the hub for service learning experiences at Emory’s nursing school.
The FWFHP is the oldest and most popular of these experiences. Each year, more than 100 student, faculty, and alumni volunteers from Emory and other state schools care for 700 to 1,000 or more Hispanic men, women, and children. This year, students also conducted health screenings for infants and children at a Migrant Head Start program and about 70 children in Tift County at Omega Elementary, a new school that requested FWFHP services.
June is an ideal time for student nurses to be in South Georgia to practice what Wold describes as “public health on the hoof.” It’s the height of the summer growing season, when farm owners employ hundreds of temporary workers, in accordance with federal visa and wage requirements, to pick eggplant, squash, cucumbers, peppers, beans, okra, tomatoes, watermelons, and cantaloupes and pack them for shipping. The men and women have no health insurance and are among the poorest of all workers in the country.
During the afternoon, students learn how to pick vegetables to experience what it’s like to be a farmworker, including removing the prickly spines from cucumbers and watching out for snakes in narrow crop rows. They visit the barracks and trailers where workers and families live; assist at Ellenton Health Clinic, a primary care facility for farmworkers; and spend time reflecting on what they learn. In the evening, students and faculty set up night camp at an area farm to provide basic episodic health care for workers. Each morning, they rise early and head to Cox Elementary in Moultrie.


A life's work

Judith Wold has been part of the Farmworker Family Health Program since it was founded by the nursing school at Georgia State University in 1994. When GSU discontinued the program, Wold brought it to Emory in 2002. This past April, Wold was honored for her longtime contributions to public health nursing and social justice—which includes the FWFHP—during an Atlanta celebration honoring the memory of Dr. Martin Luther King Jr. In 2017, she was recognized by the American Public Health Association for her work with the FWFHP.
MORNINGS AT COX ELEMENTARY
“Organized chaos” (a Judith Wold term) fills the school gym here at Cox. While a cluster of children pounce on toys and play chase, student nurses check and chart the vision, hearing, blood pressure, weight, height, body mass index, and hemoglobin level of every child. Makeshift exam rooms in the school gym afford some privacy thanks to portable screens. Adorning the screens are brightly colored sliding curtains Quinn has made to make the children feel more comfortable.

Down the hall, dental hygiene students from Clayton State University or Central Georgia Technical College do oral health exams and apply fluoride treatments and sealants to prevent cavities. Physical therapy students from Georgia State University or Brenau University work in the gym to assess children’s motor skills. University of Georgia (UGA) pharmacy students assist with paperwork throughout to update each child’s health record.
By the time the two-week FWFHP winds down, students and faculty have screened approximately 300 children from infancy to age 11. Minor health problems are the norm for most. Those who need additional care are referred to the nurse-led Ellenton Health Clinic, which serves farmworker families in Colquitt, Tift, Cook, and Brooks counties.
“We mostly see vision problems and hearing abnormalities related to earwax buildup,” says Wold. “We rarely find something serious.”
When they do, Wold and Cox Elementary staff spring into action, as they did last year for a child whom they determined had juvenile diabetes. Wold made sure that someone accompanied the child home on the bus to urge his caregiver to have him checked out immediately. A staff member from Ellenton Health Clinic also met them at the bus stop to encourage the same. But for migrant families, going to the emergency room or clinic can be difficult since time away from work can result in lost wages.

Nursing, physical therapy, dental hygiene, and pharmacy students conduct annual health screenings for children at Cox Elementary.
Nursing, physical therapy, dental hygiene, and pharmacy students conduct annual health screenings for children at Cox Elementary.
“The child was back in school the next day,” Wold says.“Routinely, copies of all of our referrals from the school go to the county school nurse who is responsible for this district. She can follow up on those kids during the year if they are here.”
Additionally, a letter written in Spanish and English is sent home to the parents of every child seen by the FWFHP to inform them about their child’s health check results.
In preparation for the FWFHP in Moultrie, BSN student Sarah Julius 18N completed a required short course in rural health, which taught her about the challenges that different populations face. As she learned, migrant children don’t always get a full year of education or have access to annual health tests and screenings because their families move around. Routine health care is more fleeting for adults. So Julius knew what to look for—anemia, diabetes, obesity, and hypertension—when screening both age groups. She also was in for a shock.
“I wasn’t expecting to see such poverty, especially working with the men at the night camps,” she says.
At Cox, Julius rotated working at different health stations, including the kids’ least favorite—hemoglobin testing—where she administered plenty of TLC. “We have to stick their fingers, but we make sure we give them cool stickers and bandages afterward,” she says.
Next year, student nurses will be able to use a bloodless hemoglobin machine, purchased with grant money awarded to the FWFHP. That means no more finger sticks to check blood for signs of anemia. “The kids will love that,” Wold says.



NIGHT CAMP AT LEWIS TAYLOR FARMS
Late each day, after a quick bite of supper, students and faculty line up their cars in the Moultrie Hampton Inn parking lot for the 30-minute drive to set up night camp at Lewis Taylor Farms. As the drivers head out on U.S. Route 319, Quinn leads the way in her white van, while Wold brings up the rear in her big blue pickup. After a few miles, the caravan turns left off the highway, then left again, then right. It has rained a lot during the past few days, and the dirt road is muddy and slick, so the drivers take it easy.
When the caravan finally arrives at the barracks where farmworkers live, dozens of Hispanic men, dressed in shorts, T-shirts, and sneakers or flip flops, are waiting. The students quickly set up triage and treatment stations outdoors in the grass in the warm, humid air. Bug spray and Emory Nursing hand fans are standard issue for their work.

Now in their second week of the FWFHP, students are comfortable with the routine. Experience is in their favor when lightning flashes across the darkening sky, prompting nursing faculty member Elizabeth Downes o4MPH to make a safety call: “Okay folks, move inside.”
Unfazed, the students pick up tables, chairs, papers, and supplies and move them into a screened cantina and rec room and set up their stations again. “Holy cow,” says Wold, calmly eyeing the scene.
The cantina is hotter and more crowded than being outdoors, but the students and faculty settle in and resume work. Their young and middle-aged patients wait quietly, standing or sitting where they can.
One by one, the men are checked in, and faculty and students triage them according to their needs. One worker from Mexico has asthma and receives an inhaler, with instructions to go to Ellenton Health Clinic if he’s not any better in two weeks. Another worker complains of an earache, and a nurse practitioner student irrigates his left ear to provide some relief.
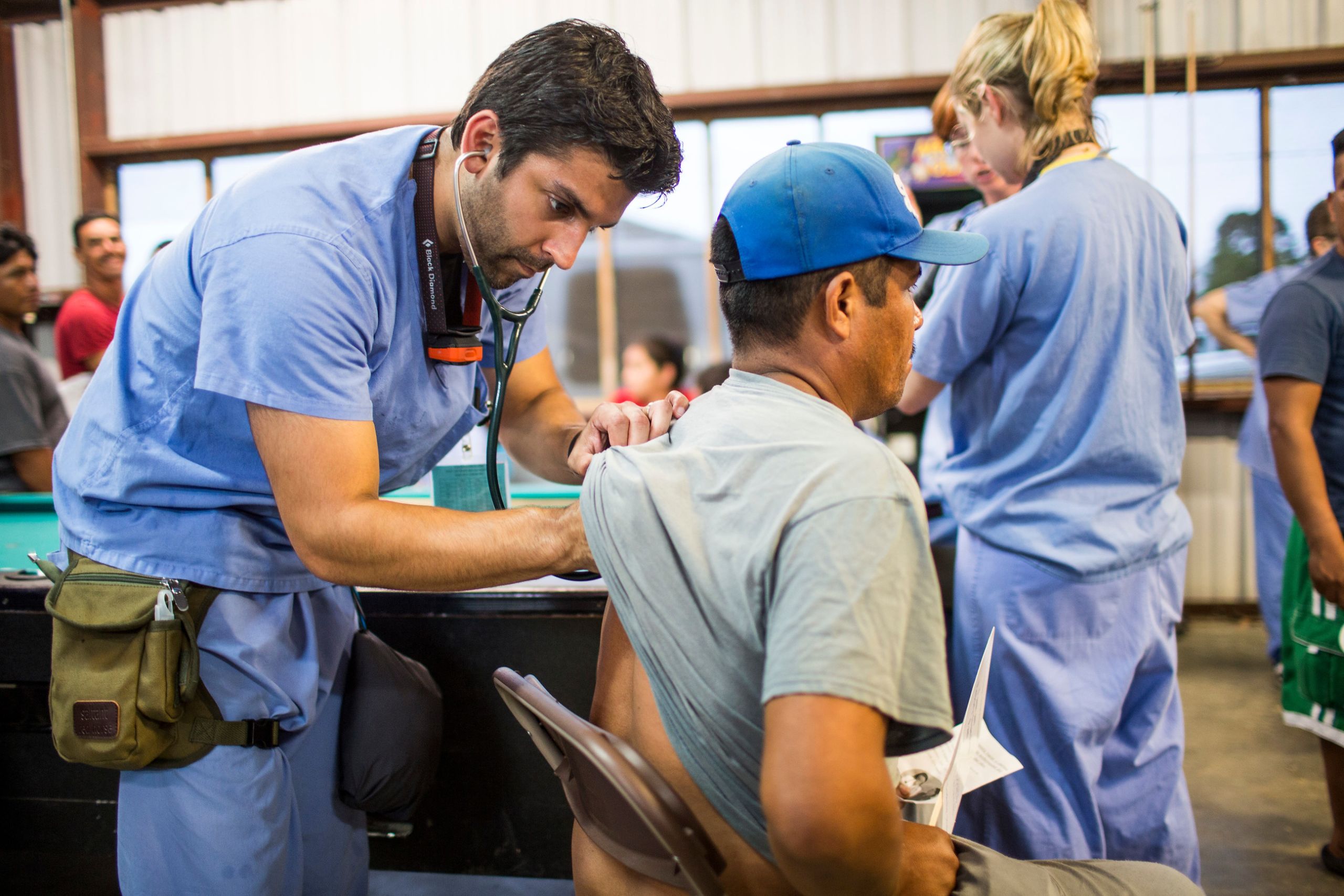
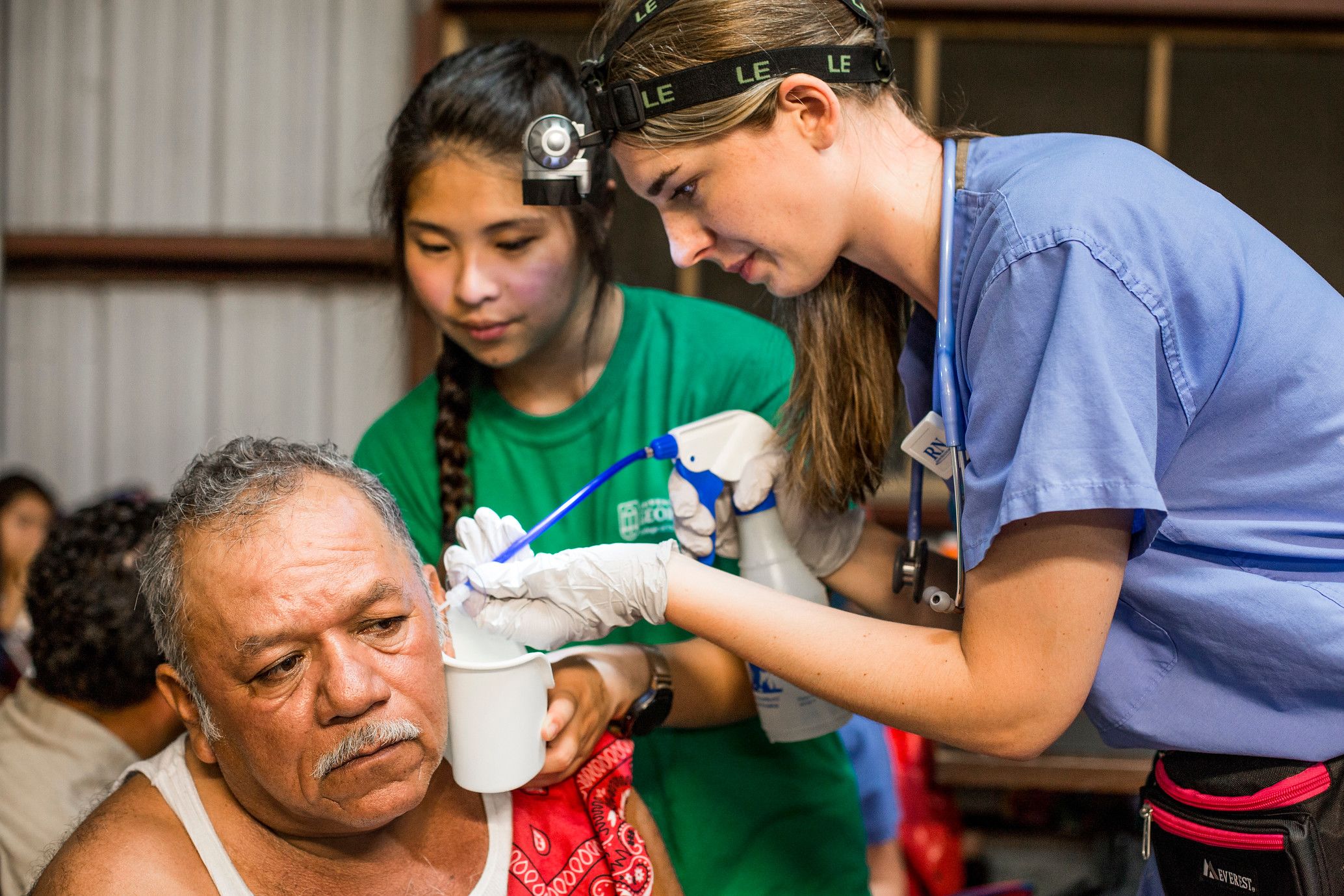
Migrant workers often receive health care for the very first time at night camps on farms near Moultrie.
Migrant workers often receive health care for the very first time at night camps on farms near Moultrie.
At 26, Carlos Romero is younger than most of the men. He has come to Georgia for the third time to work and send money to his wife in El Salvador. Bending down and up to pick crops for hours at a time has brought on his back pain and headache. After a nurse practitioner student assesses him, a pharmacy student gives him over-the-counter medication and analgesic cream for his lower back.
“Is this your only opportunity for health care?” an interpreter asks Romero. “Si,” he replies.
Emeka Anosike 18MSN, a family nurse practitioner student, has gained a lot of insight at night camps such as this. He has learned to navigate the language barrier aided by Spanish interpreters. He has come to understand the physical problems the men have because of their work. And he has learned something else.
“This camp has been rewarding in that it’s an interprofessional effort involving students studying to be nurses, pharmacists, physical therapists, and dental hygienists,” says Anosike. “One thing I’ve learned from the physical therapist students is how to educate the men on proper ways to bend and pick up things and proper body mechanics. All of those things can help alleviate the musculoskeletal issues they have.”
The students’ efforts can backfire. At one of the night camps, Anosike advised a man to eat more fruits and vegetables to supplement his diet of tortillas and beans. But when he shared a meal with men at the camp, there were no fruits or vegetables on his tray.
“How could I tell someone to eat fruits and veggies when those things aren’t available,” Anosike says. “If I’m advising someone, I need to understand where they’re coming from. I need to understand their social constraints, their economic barriers, to be able to provide education and advice suited to that individual.”
Floating among Anosike and other students is Lissette Badillo, a volunteer interpreter whose parents came from Mexico as migrant farmworkers. Badillo spent childhood summers at Lewis Taylor Farms, where her parents worked in the fields. Her family moved with the harvest seasons in Florida, Georgia, and Kentucky, where her parents picked tobacco. No one told them about tobacco poisoning, which caused their nausea, vomiting, and exhaustion.
During the night camps, students and faculty offer health education to farmworkers on a variety of topics: proper foot care, staying hydrated, sun and mosquito protection, preventing sexually transmitted diseases, eating less sugar and salt to guard against diabetes and hypertension, and reducing or avoiding use of tobacco and alcohol.
Badillo is heartened by the services that Emory’s Farmworker Family Health Program provides. “I’m thankful that these services exist to provide some health care to the field workers,” she says. “When I was younger, they weren’t available. Simple health education can go a long way.”


ELLENTON HEALTH CLINIC
A fixture at each night camp is the Ellenton Health Clinic mobile unit, where Emory nurse practitioner (NP) faculty and students conduct more thorough physical exams and UGA pharmacy students give out antibiotics (prescribed by NP faculty) for workers who need them. Those with chronic or serious conditions are referred to the actual clinic for follow-up. For some of the workers, the FWFHP marks the first time they’ve received basic health and dental care.
“The night camps help a lot of the people who have been here a short time,” says Cheryl Kicklighter, the nurse practitioner who directs Ellenton Health Clinic. “They’ve come from another country. They don’t speak the language. They don’t know what to do if they have a health problem. The Emory program lets them see there are people interested in caring for them and there is a place they can go when they have a health need. It opens the door for them.”

Above: Emory nurse practitioner students help assess a patient at Ellenton Health Clinic. Left: Farmworkers built this chapel outside their barracks at Lewis Taylor Farms.
Above: Emory nurse practitioner students help assess a patient at Ellenton Health Clinic. Left: Farmworkers built this chapel outside their barracks at Lewis Taylor Farms.
Located about 10 miles from Moultrie, Ellenton Health Clinic annually serves just over 3,000 unique patients (which translates to about 6,000 patient visits). It is one of six clinics, operated by the Georgia Department of Community Health with federal funds, specifically for farmworkers. Patients pay for all of their services.
“Our patients pay so well that we don’t have a billing system,” says Kicklighter. “These are not people who are looking to get an excuse from work. They are looking to get well so they can get back to work as soon as possible. They respect what we tell them and try to do it.”
Clinic patients receive care for work-related injuries (such as hand wounds from cutting greens and cabbages) and muscle fatigue, colds and flu, and chronic conditions. Nurse practitioners at the clinic see high incidences of asthma, hypertension, and diabetes—a prevalent condition among Hispanics related to diet and genetic predisposition. Patients with cancer and other serious illnesses are referred to area doctors and hospitals for treatment. If requested, clinic outreach workers help ill farmworkers get to Ellenton to be seen.

Clinic nurses also focus on women’s health, including prenatal care. The clinic’s popular centering pregnancy program has helped decrease the number of low-birthweight babies born to Hispanic women in the area.
Some Emory student nurse practitioners and faculty spend a day at Ellenton Health Clinic to assist with women and family practice patients. A few years ago, students sought Kicklighter’s advice on what they could do for their annual Moultrie project. “We need boots!” she told them.
Students now collect money to purchase rubber boots (about $15 a pair) and distribute them to men at night camps every year. The boots protect workers’ feet from chemical burns caused by standing in wet fields treated with fertilizer and insecticides.
“We have an excellent relationship with area farmers,” says Kicklighter. “They appreciate the fact that we come out at night and provide health services for their workers. We try to meet as many of the workers’ needs as we can because they just don’t have the resources to go anywhere else.”
A SENSE OF PURPOSE
When the nursing and other students first arrive in Moultrie on a Sunday, they go on a scavenger hunt to learn the layout of the town. That first evening, the mayor and other residents welcome them at a dinner held at the Colquitt County Center for the Arts. Over the next two weeks, 50 church volunteers provide lunches for all of the students and faculty. After the FWFHP ends each year, Wold writes more than 100 notes to thank everyone who helps with the program. “Everyone in the community is important to this partnership,”she says. “We want to be welcomed back next year.”
No one understands the impact of the FWFHP more than Wold. In Colquitt County, the growing season is year-round, and the roughly 300 farms there raise more agricultural products than any other Georgia county.
“If there’s food on your table, thank a farmworker,” says Wold, who will return to Moultrie next year as an emeritus professor. “If we did not have farmworkers, we would be paying $10 for a tomato or cucumber. They are vital to our economy. We need them, and they need us.”
By Pam Auchmutey | Photos and Video by Ann Watson



Poetic Service
Taking Medicine to the Fields of South Georgia
About an hour's drive south of Moultrie, the program led by the Physician Assistant (PA) Program in the School of Medicine provides free health care to migrant workers at outdoor clinics on farms in and around Valdosta and Bainbridge.

The South Georgia Farmworker Health Project (SGFHP) began in 1996 with eight PA students, three PA faculty, and one physician, all under the direction of Tom Himelick, then a faculty member in the PA Program.
Today, the SGFHP is a multidisciplinary effort involving some 200 students, clinicians, interpreters, and logistics volunteers who come together each summer to continue the work that Himelick began. Now led by faculty member Erin Lepp, the SGFHP has become the hallmark initiative of the PA Program and received local, regional, and national recognition for its innovative, culturally appropriate delivery of care. Like the nursing school’s program, the SGFHP helps address the health care needs of an often-overlooked population—migrant farmworkers.
When farmworkers pick bell peppers, they fill their baskets again and again to earn more money. The repetitive work often causes back aches and muscle strains.
When farmworkers pick bell peppers, they fill their baskets again and again to earn more money. The repetitive work often causes back aches and muscle strains.
While fruit and vegetable cultivation in Georgia brings more than a billion dollars a year into the state, pickers typically receive low pay, live in barracks or temporary housing, and have limited access to routine medical and dental care, prenatal care, and medications.
Over the past 22 years, SGFHP clinical teams have treated a range of patients, including people who have never been seen by a provider, women in labor, and workers with acute and serious chronic illnesses. Each June, the rotating morning and afternoon clinics provide free care for 1,800 or more farmworkers and their family members over 12 days. Teams see an additional 300 workers during an October weekend clinic.
The clinics are staffed primarily by Emory PA students, faculty, and clinicians and assisted by Emory physical therapy and medical students. Emory also partners with the PA Program at Mercer University, family therapy students from Valdosta State University, nursing students from Bainbridge College, and medical students and faculty from the University of Georgia and Morehouse University. Spanish and Creole interpreters from Atlanta, South Georgia, and Florida volunteer as well.

During the clinics, farmworkers receive a hygiene kit with donated items, such as a toothbrush, toothpaste, condoms, washcloths, and work gloves. They also receive a clear pair of UV-blocking glasses to help prevent pterygium, a benign callus on the eye occurring in people who spend a lot of time outdoors. Most farmworkers don’t wear sunglasses because they distort color perception and make it difficult to determine when crops are ripe for picking. The clear glasses allow them to see color clearly while protecting their eyes.
During the 20th anniversary celebration of the SGFHP in 2016, then U.S. Poet Laureate Juan Felipe Herrera recounted how growing up among California farmworkers in the 1950s shaped much of his poetry. Among the stories Herrera shared was how his father left their home in Mexico and jumped on a train to begin a new life in the United States. “Jump on that train” became a family motto that his father repeated during hard times.
“You meet the people you serve at a difficult time, providing amazing, lifesaving services and information,” Herrera told SGFHP students, faculty, and volunteers. “These are things we do not get in our communities. You not only bring health, well-being, and happiness, but you also bring us unity.”
By Jodie L. Guest 99PhD 92MPH | Photos and Video by Physician Assistant Program Faculty and Students







ON HOLY GROUND
by Tom Himelick for the 20th anniversary of the
South Georgia Farmworker Health Project

SGFWP founder Tom Himelick
SGFWP founder Tom Himelick
Briefly we stood on holy ground
At the intersection of the ways of
justice and medicine
Georgia’s black loam was green
shrouded to the horizon
We listened
Briefly we heard the soft voices
of children in the field
Picking replacing their
childhood hours
Fatigue in their eyes
We heard the horrors of the
desert crossing
Of friends gone
No más muertas no más muertas
No more deaths
Briefly we saw men and women
old beyond time
Hopeless years away from
their families
Briefly we felt the merciless
sun and later retreated to our
air conditioning
And our insulated lives
Briefly we were called angels
The worker looking down at his ragged shoes
Thanking us for being there
between fields
For caring for his hermanos
y hermanas
But we knew who the real
angels were
Whose sacrifices fed us without
our gratitude
Briefly we stood between cars
and wept in darkness
For the injustice
For the little we could do
For the understanding
of our complicity
For memories that will
continue to haunt us
Briefly tonight we gather
to remember
To celebrate
And to affirm
That justice and equity will
not be brief
That with these hands
That with these hearts
Estos corazones
We can change

Need to know more?
Please visit Emory Nursing Magazine, Emory Physician Assistant Magazine, Emory News Center, and Emory University.