Sara's Journey
A baby in need of complicated surgery. A medical student volunteering in Haiti. A chance for a better life.

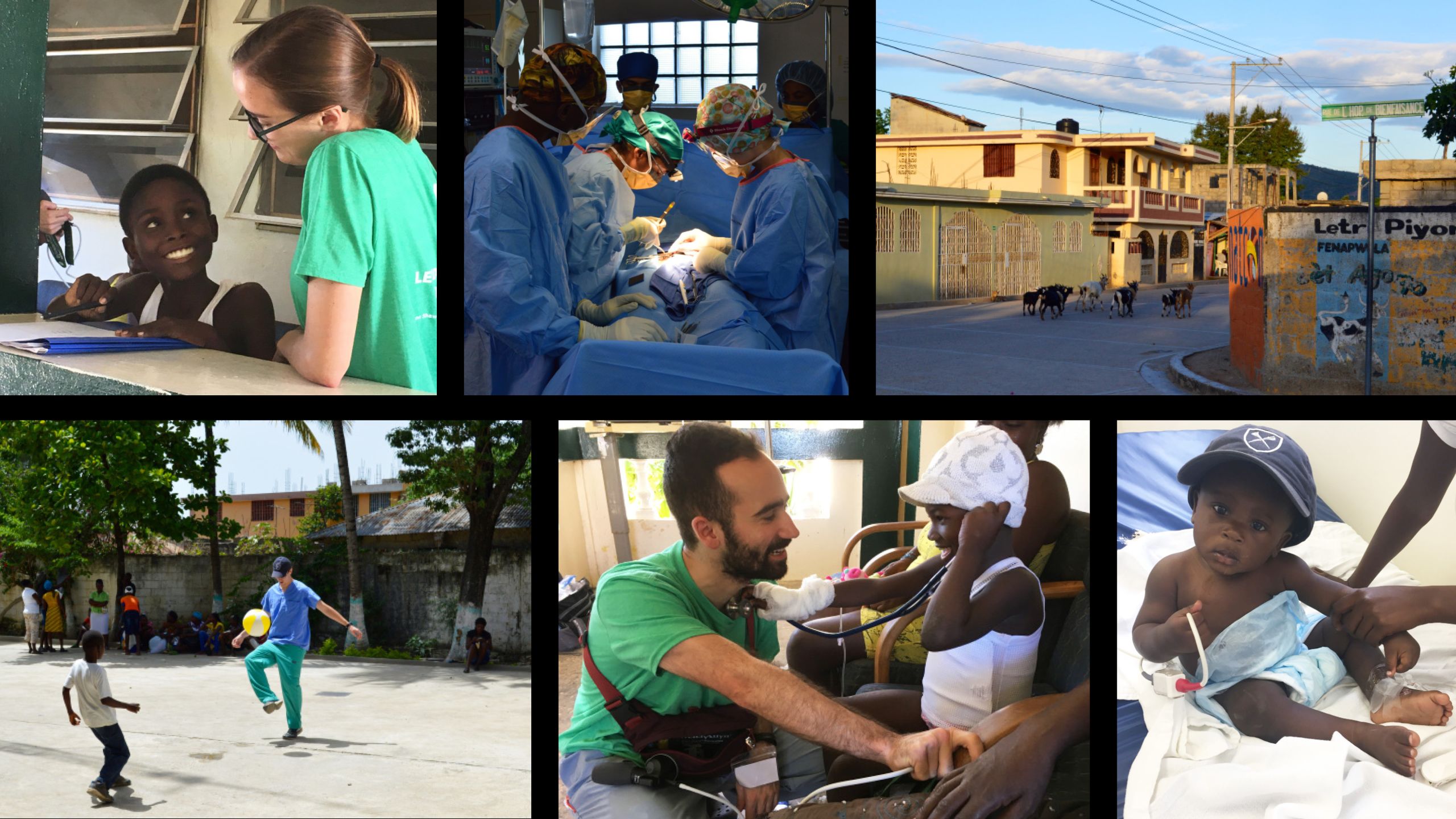
DOZENS OF PEOPLE a day streamed into the hospital to see the medical volunteers, having heard about the clinic on the radio or by word of mouth. Some traveled two and three hours to get there, over dirt roads and on crowded buses. They came from rural villages and the capital city of Port-au-Prince, carrying sick babies or supporting elderly relatives.
Haiti, already one of the poorest countries in the world, had been further devastated by the 2010 earthquake. Most of its 10.5 million residents live on less than $2.50 per day, and medical resources and staff are scarce. The quake demolished 50 health centers and the ministry of health.
The Emory Haiti Alliance (formerly Emory Medishare) has organized a surgical trip to the island each summer for more than a decade—with volunteer surgeons, anesthesiologists, medical students and residents, and nurses providing free care at Hospital St. Therese in the Central Plateau, the most medically underserved area of Haiti.
“The clinic experience for all physicians is invaluable. It is the essence of the bond physicians form with their patients. A common misconception is that surgeons would just as soon never have clinic. On the contrary, it is the clinic setting that allows us to first meet patients and understand their chronic surgical disease so we can better determine how to help them. It also allows us to learn from our own attempts to cure disease so we can perfect our decision making and operative approaches over time. This is no different in Haiti. For the students, interacting with patients in Haiti who are coming from far away allows them the opportunity to better understand the inherent barriers to care, and how we can best overcome those barriers. It allows them a window of insight into the serious weight we take on our shoulders when making decisions that can change the course of an entire individual’s life, and that of their family. In short, it matures students quickly and helps them understand the serious professional commitment they have made by becoming doctors, regardless of the specialty they ultimately choose.”
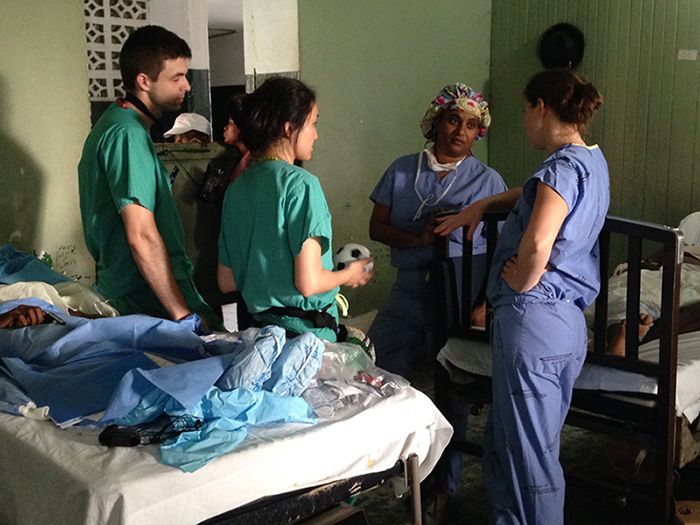
Dr. Jahnavi Srinivasan consults with colleagues on the Emory surgical trip to Haiti. Photo courtesy of Emory Surgery
The month-long trips combine student education with care, and the medical teams perform multiple surgeries each day, seeing more than 100 patients in all. Medical students assist surgical residents and faculty, who bring their own supplies and face challenging conditions: minimal running water, ORs that function on a diesel generator, intermittent power outages, operating by headlamps.
In 2016, medical student Justine Broecker was in Haiti volunteering with her father, Bruce, a pediatric urologist and Emory adjunct faculty member. “With two parents who are physicians, I had been exposed to medicine my whole life,” she says.
One of the local Haitian doctors, Rony Destine, a program manager with Project Medishare, had hopes that surgeons at the clinic could help an infant he had encountered in Port-au-Prince with a rare birth defect. The child, Sara, and her mother, Michel-Ange, had traveled to the clinic. “I was with my dad when he was examining Sara, who was just three months old,” says Broecker. “My dad recognized the disorder—bladder exstrophy.” Sara’s bladder was on the outside of her abdomen, and she didn’t have normal closure of her abdomen and pelvis. The disorder requires a complex repair involving both urologic and orthopedic surgery. Typically, in the U.S., bladder exstrophy is recognized in utero or directly after birth and repaired within a few days or weeks. But the clinic’s team lacked a pediatric orthopedic surgeon and proper equipment. “It was beyond what we could do at that hospital,” says Broecker.
Delaying the repair can be hazardous to an infant’s health, with risks of inflammation and infection, and the longer it takes, the more difficult closure becomes. “It was pretty disheartening,” Broecker says. “We couldn’t make any promises. But it was difficult to give Sara this diagnosis and then tell her mom we couldn’t do anything to fix it.” Upon her return to Emory, she started making calls and mobilizing support to bring Sara and Michel-Ange to Atlanta for the repair. “The surgeons had volunteered their time, but we didn’t have a way to pay for visas and travel, or a place for Sara and her mother to stay,” Broecker says.
Willy Blain, an anesthesia technologist and a member of the Emory Haiti Alliance team of Haitian origin, helped to translate for patients, and stayed in contact with Sara’s family. But when Hurricane Matthew hit Haiti as a Category 4 storm in October 2016, the country was again pitched into chaos. “We lost contact with Sara’s mom after the hurricane,” Broecker says. Their old phone number didn’t work and no one had an address for them.
Broecker had gotten in touch with the charity Childspring International, which was offering to pay for travel, help with logistics, and arrange for a host family in Atlanta. Best of all, Childspring representatives in Haiti managed to locate Sara and her mother and reinitiate contact after the storm.
Broecker and the host family met Sara and Michel-Ange at the airport on February 11, 2017. Sara was initially scheduled to have surgery right away but wasn’t well enough. She had a cold and was malnourished and anemic. “The decision was made to delay the surgery and let her gain more strength,” Broecker says. “I was pretty happy to see her. It was all a little surreal. When we first encountered them in Haiti, I didn’t think any of this would be possible. I was grateful to see everyone’s hard work pay off, but getting her here was just the first step.”
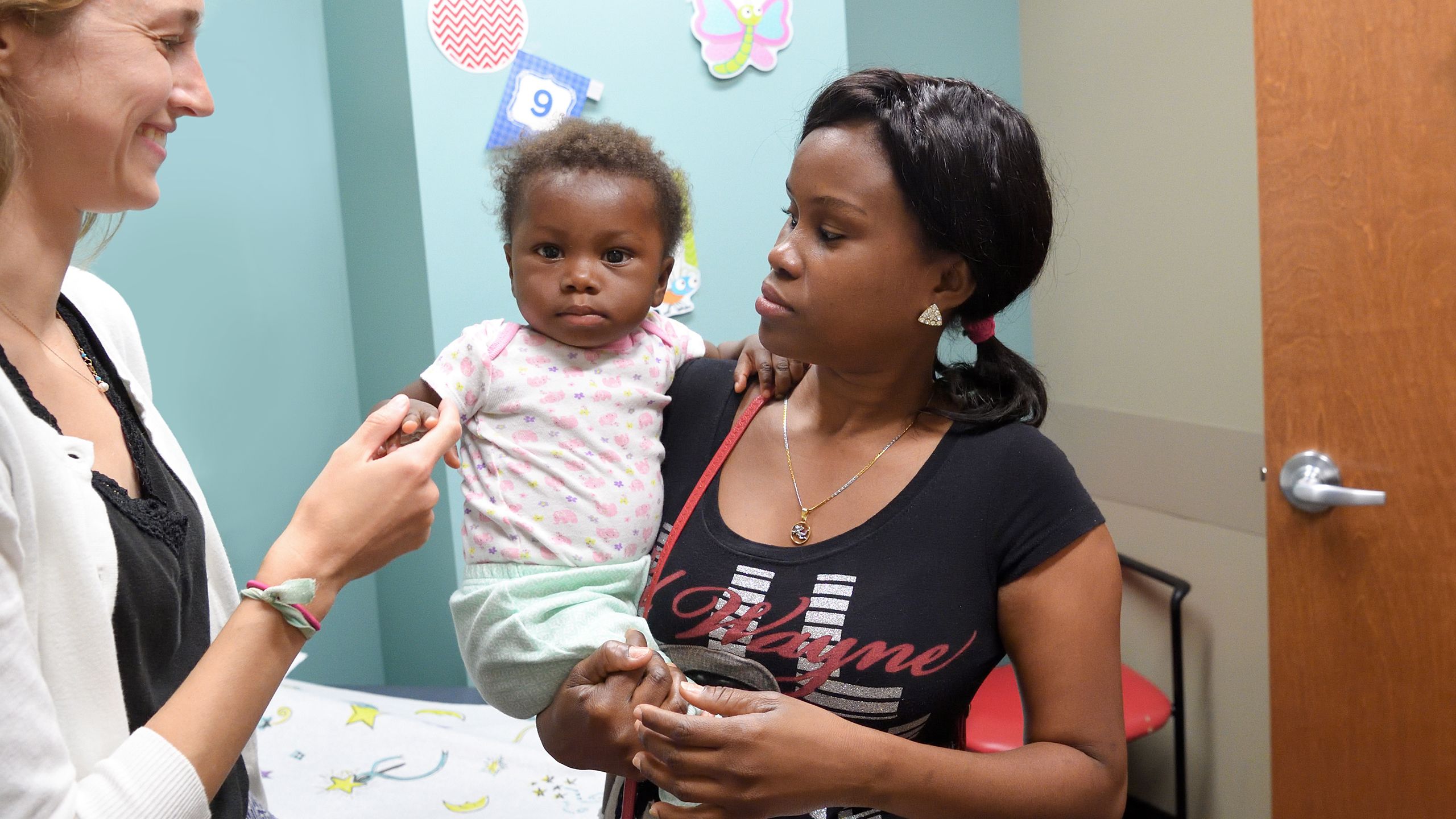
At Childspring International’s annual gala at the Ritz Carlton Downtown in Atlanta the following month, 11-month-old Sara and her mother, Michel-Ange, were special guests. Childspring holds the event to raise funds for surgery for children from all over the world.
Sara, a bundle of energy, spent much of the night in the foyer crawling around on the carpet in her leggings and white party dress. Michel-Ange, who spoke through a volunteer interpreter from Atlanta’s Haitian community, said Sara’s father had died when the baby was 2 months old; her three older children were staying with relatives in Haiti. “Sara is my heart,” Michel-Ange said. “I asked God not to let me lose her. She was meant to be here.”
Physicians Brad and Laura Lord were their local host family. Laura Lord, a neonatologist, was at the gala, where Sara bounced happily from person to person all evening. “I thank them for opening their home and heart to us,” said Michel-Ange.
Sara went into surgery on April 21, 2017, at nearly a year old. Broecker was invited to scrub in, with pediatric orthopedic surgeon Robert Bruce and pediatric urologic surgeon Edwin Smith. “It was a great opportunity, since it’s such a rare disease,” she says.
“Sara is my heart. I asked God not to let me lose her. She was meant to be here.”
“Justine had sent images to us and given us a bit of the history and Sara’s medical condition,” Smith says. “She was the bedside identifier of the problem and started the ball rolling.”
Bladder exstrophy occurs in about three of every 100,000 births. Smith’s group sees three to four cases a year, since they have expertise in dealing with the disorder. “It used to be that we would rush to close the infant’s bladder during the first three days, to take advantage of the effect of maternal estrogen and the malleability of the pelvis,” he says. “But then we discovered there is some flexibility.”
The congenital birth defect, while not fatal if unfixed, does carry a social stigma—and the surgery is the first step toward continence. “If you look back in medical archives, patients can live for many decades with bladder exstrophy, but it makes you more prone to bladder cancer at a younger age,” Smith says. “And other conditions attend it, such as uterine or rectal prolapse. Other pelvic structures are unsupported because pelvic muscles are not in the right position.”
Sara, in fact, did have rectal prolapse. Bruce started off the procedure with an osteotomy, a controlled break in the iliac bones—the upper crest or “wings” of the pelvic girdle. The pelvis was opened and the pubic bones separated. “This hinges the bones, allowing the pelvic bones to meet in front of the bladder, and puts the muscles in a better position to support the bladder,” Smith says.
The careful dissection of the bladder neck area is critical, Smith says, as is the closure of the bladder neck and urethra, and sinking them down behind the pubic bone and within the pelvic muscles. When a bladder forms on the outside, it may be deficient in a variety of ways—smaller, less elastic, or not of normal innervation—which can make the outcome less desirable. “We try to do as limited a dissection as possible, yet securely close the bladder, pelvis, and abdomen,” Smith says. “You don’t want to lose nerve or blood supply to the organ. That’s part of the art of doing this.”
The operation went smoothly, he says: “It was a coordinated effort with urology, orthopedics, anesthesia, and pediatrics—a multidisciplinary team makes a good result much more likely.” The doctors put Sara in a suit of pants made of casting material, a critical step to stabilize the pelvis while adding to the security of the surgical closure. The team has about 60 bladder exstrophy patients they follow long-term.
“I’ve personally seen how well these kids can do. We’ve cared for infants that grew up to become a high school cheerleader and an All Star second baseman,” Smith says. “They can have very normal lives.” Some patients’ bladders function normally after the initial operation, while others need additional surgeries.
“It was all a little surreal. When we first encountered them in Haiti, I didn’t think any of this would be possible.”

Broecker, now a surgical resident at Emory, was busy with medical school graduation right after the surgery, but had the chance to visit a few more times with Sara and her mother before they left Atlanta. Sara was out of her cast and doing well. “Sara’s situation made an impression on me from our first meeting in Haiti,” Broecker says. “I realized her mother’s determination to do anything and everything to help Sara get the operation. That inspired me to do everything I could to help her as well.” EHD