|  | |
 |
| Stay home and stay safe | So many of our Woodruff Health Sciences Center colleagues and community members are asking how they can help our courageous health care team.
Allies such as the Alliance Theater, our own co-workers, and our neighbors are helping to sew masks to aid with critical shortages in personal protective equipment. And you may have seen the heartwarming video of Atlanta residents on their porches and balconies cheering for the city’s health care workers every day at shift change—a touching show of solidarity and gratitude that is much appreciated and very well deserved.
Of course, the very best way to help is by staying home and helping us flatten the curve. I urge you to follow strict social distancing guidelines which will curtail the spread of the virus and give our health care colleagues a fighting chance. They’re on the frontlines putting themselves and their families at risk to save lives. Slowing the spread of the disease is something we can all do to help them.
Thanks for all you are doing to encourage and support our health care team and to help them stay safe.
Please direct questions and comments to evphafeedback@emory.edu.
Jonathan S. Lewin, MD, FACR
Executive Vice President for Health Affairs, Emory University
Executive Director, Woodruff Health Sciences Center
CEO, President, and Chairman of the Board, Emory Healthcare | |
| |
| 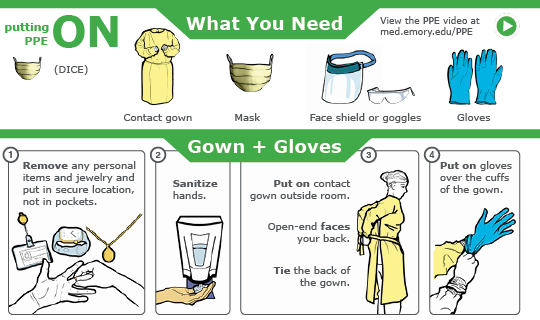 | Coronavirus behind-the-scenes efforts | How should health care workers deal with the shortages of personal protective equipment (PPE) when treating Covid-19 patients? Emory’s Visual Medical Education team and Library and Information Technology Services (LITS) assisted the School of Medicine and Emory’s Serious Communicable Diseases Program to provide an answer. In an amazingly short time, they created a set of graphics and videos that instruct medical personnel on the use of PPE in two scenarios—when there is an adequate supply of PPE and when there is a shortage. The site can be found at med.emory.edu/PPE.
The site resides in the National Emerging Special Pathogen Training and Education Center (NETEC), which was created after the Ebola epidemic five years ago to share lessons learned. The NETEC Resource Repository was created by LITS and provides free access to a database of up-to-date education and training resources, including webinars, online courses, research articles and printable posters to help train and prepare U.S. health care facilities for emerging threats.
The behind-the-scenes story of the site creation is a testament to what can be accomplished when everyone works together, according to Michael Konomos, visual medical education team leader for the School of Medicine. No sooner would the team finish filming and editing a video—a task they did in days rather than weeks—than they needed to reshoot. “It seemed like every 12 hours the protocols would change because we were running out of something else, so we’d have to reshoot to reflect that,” says Konomos. “It felt like the legend of Sisyphus. Each day we had to roll that boulder back up the hill. But we all knew how important it was, so we kept rolling that thing as fast as we could.”
It was a true team effort. “Sonia Bell led the Serious Communicable Diseases Unit (SCDU) efforts,” says Konomos. “Sharon Vanairsdale and Kari Love, nurse leaders in SCDU and Emory Healthcare Infection Prevention, were in all the discussions about protocols and would approve the work or offer corrections before it went out. Steve Bransford from Emory Center for Digital Scholarship shot almost all of the video with SCDU lead nurse Josia Mamora. VME’s Satyen Tripathi and Bona Kim did flyer production and video editing, and health care providers allowed us to film them doing the training. Months of work was accomplished in a matter of days because everyone was willing to pitch in and do whatever it took.”
The team actually shot the first video in the SCDU, since Emory had not yet admitted any Covid-19 patients. By the time they returned to shoot another version a few days later, the hospital was full, so they had to film in the clinic, turning an exam table into a hospital bed.
“Institutions around the country and in the military are using the site regularly, and checking back in when we have updates,” says Konomos. “Veterans Affairs requested the build files to modify for their purposes. Grady did the same, since they have PPE. We’ve had 8,000-plus views in the last week. People are viewing the pages from as far away as Brazil, Mexico and Canada.”
NETEC Resource Repository is distributing other Covid-19 related materials, according to Bell. Mark Caridi-Scheible (anesthesiology) and NETEC colleagues from other institutions presented a webinar on lessons learned so far in the critical care of Covid-19 patients. Jill Morgan (advance respiratory ICU) participated in a webinar regarding PPE conservation and decontamination. And Anna Quay Yaffee (emergency medicine) and David Wright (emergency medicine) will lead a webinar on Covid-19 in the emergency room. | |
| |
| 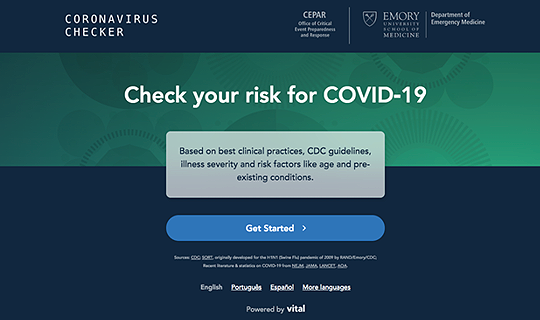 | Self-triage tool for Covid-19 | Addressing a critical need, our doctors have helped create a new online tool allowing people everywhere to assess how likely it is that they have contracted the novel coronavirus.
C19check.com makes it easy for the general public to self-triage and is designed, in part, to prevent a surge of patients at hospitals and healthcare facilities.
The site was built at Emory’s Health DesignED Center with Alex Isakov (Office of Critial Event Preparedness and Response), David Wright (emergency medicine), Anna Quay Yaffee (emergency medicine), and Justin Schrager (emergency medicine). It is powered by Vital, an ER management tool launched last year by Schrager and a partner. With the rise of COVID-19, Schrager and his partner foresaw an overload of ERs worldwide. They sought a tool to help patients better self-triage before burdening hospitals and found none. They diverted all of Vital’s resources into building C19check.com.
“We’re all fighting, in ways big and small, to keep our loved ones out of harm’s reach. But the anxiety and uncertainty around the best way to do that can result in crowded emergency departments that will have difficulty managing the surge,” says Schrager. “Our goal with C19check.com is to prevent that from happening, while also making it super simple for people to understand and follow CDC guidelines.” Read more about C19check.com’s development. | |
| |
|  | DRIVE joins partnership to test coronavirus drug | Drug Innovations at Emory (DRIVE) is partnering with a Miami-based biotechnology company, Ridgeback Biotherapeutics, to rapidly take an experimental drug it developed to human trials. The drug, EIDD-2801, which is now being tested as a treatment for Covid-19, has shown promise against a number of other diseases, including influenza, SARS, MERS, chikungunya.
“With EIDD-2801 close to entering clinical trials for influenza and its activity against the SARS and MERS coronaviruses, we immediately recognized that EIDD-2801 had the potential for treating COVID-19. Based on our extensive testing, we believe EIDD-2801 will be effective in treating individuals that have been sickened by COVID-19," says George Painter, director of the Emory Institute for Drug Development and CEO of DRIVE.
"Given Ridgeback Biotherapeutics' experience in accelerating the development of potential therapeutics in outbreak settings and its proven commitment to global health, we are confident that Ridgeback can quickly advance EIDD-2801 into clinical trials for COVID-19 and initiate steps toward ensuring a rapid development path for this promising drug," says Painter.
Ridgeback Biotherapeutics has unique experience meeting the challenges of developing novel drug treatments during an ongoing disease outbreak. In 2018, at the beginning of the Ebola outbreak in the Democratic Republic of the Congo, the company licensed a promising Ebola therapeutic, for which it is currently seeking commercial licensure. Read more about the DRIVE/Ridgeback partnership. | |
| |
|  | Emory new site in NIH-sponsored coronavirus vaccine study | Emory’s Vaccine and Treatment Evaluation Unit (VTEU) is participating in a clinical trial testing a vaccine for the prevention of COVID-19, the first such vaccine to be tested in the United States.
The goals of the Phase I study, which began on March 16 at the VTEU at the Kaiser Permanente Washington Health Research Institute in Seattle, are to test whether the investigational vaccine is safe, and how much it stimulates the immune system. If the vaccine is found to be safe, future studies will examine whether it can prevent infection.
The study is sponsored by the National Institute of Allergy and Infectious Diseases (NIAID), part of the National Institutes of Health. The Emory VTEU is part of NIAID’s Infectious Diseases Clinical Research Consortium supporting this trial. Emory has been a VTEU site since 2007.
The principal investigator for this study at Emory is Evan Anderson, and Nadine Rouphael is serving as the Emory VTEU contact principal investigator.
The vaccine is called mRNA-1273 and was developed by NIAID and Moderna, Inc. The vaccine is based on messenger RNA, which tells some cells in the body to make a viral protein. The RNA-based approach allows for faster vaccine development than older methods. The vaccine does not contain coronavirus itself and cannot cause infection.
The trial aims to enroll 45 participants total across the two sites. Participants must be adults in the Atlanta area age 18 to 55. To be eligible, they can’t have chronic diseases or health conditions that affect the immune system, and they can’t be taking immunosuppressive medications. Other criteria and additional information about the vaccine study are available at ClinicalTrials.gov. | |
| |
|  | | Virtual Match Day | Instead of tearing open envelopes, fourth-year medical students learned where they will go for post-graduate training via a special email that hit inboxes promptly at noon on March 20. Of the 138 Emory medical students who participated in Match Day, 36 will spend all or part of their residency training in the state of Georgia; 31 will begin their training at Emory, and 30 will remain at Emory for their entire residency. In addition to Emory, the students will receive their residency training at other prominent institutions including Duke, Harvard, Baylor, University of California San Francisco, University of Chicago, University of Washington and others. Read more here.
| | |
| | |  | | EJCH receives Magnet recognition | Emory Johns Creek Hospital has received the prestigious Magnet recognition by the American Nurses Credentialing Center’s Magnet Recognition Program. The recognition is the most esteemed honor given to a health care organization for nursing excellence and patient outcomes. Pictured above at the Magnet Pep Rally in January, l-r: Marilyn Margolis, EJCH CEO; Sharon Pappas, chief nurse executive for Emory Healthcare; Heather Redrick, EJCH CNO; and Trina Geyer, EJCH Magnet Recognition Program manager and manager of nursing support operations.
| | |
|
| |
|  | | Three Emory hospitals named top in Georgia | Three Emory hospitals have been named as top Georgia and US hospitals in Newsweek’s list of World’s Best Hospitals 2020, which ranks more than 1,500 leading hospitals in 21 countries. In Newsweek’s “Best Hospitals – USA” list, hospitals are ranked nationally and by state. In Best-in-State rankings, Emory University Hospital ranked 1st place, Emory Saint Joseph’s Hospital ranked 2nd place and Emory Johns Creek Hospital ranked 3rd placed in Georgia. Nationally, Emory University Hospital ranked No. 22, Emory Saint Joseph’s Hospital ranked No. 93 and Emory Johns Creek Hospital ranked No. 197.
| | |
| | |  | | Tweet from Barack Obama | Rachel Patzer (surgery) recently shared a series of Tweets urging the public to take the Covid-19 epidemic seriously as her ER doctor husband is forced to self-quarantine. Patzer’s husband is currently treating coronavirus patients, and the family made the decision that he would isolate and move into their garage apartment for the foreseeable future. Since posting, she has been retweeted more than 59,000 times. Most notably, President Barack Obama replied to Patzer’s Tweets, saying “We owe a profound debt of gratitude to all our health professionals and everybody who’ll be on the front lines of this pandemic for a long time. They’re giving everything. May we all model our own behavior on their selflessness and sacrifice as we help each other through this.” Patzer was also interviewed on CNN, where she discussed her husband’s sacrifice to protect herself and their three children from the virus.
| | |
|
| |
| |  | | Matthew Clifton has been appointed chief of Division of Pediatric Surgery. He has served as interim chief for more than two years.
Craig Coopersmith was inducted as a Master of Critical Care Medicine of the American College of Critical Care Medicine. This is the highest designation one can have in critical care.
Sheryl Gabram-Mendola is transitioning from her clinical role in the Department of Surgery as well as her leadership positions and clinical work at Grady Memorial Hospital as surgeon-in-chief, chief of the Division of Emory Surgery at Grady, deputy director of the Georgia Cancer Center for Excellence at Grady, and director of the Avon Comprehensive Breast Center at Grady as of April 16th, 2020, with planned retirement to Emory Emeritus Professor in January 2021.
Peng Jin has been appointed chair of the Department of Human Genetics. Jin has served as professor in the department since 2013 and vice chair since 2016.
Amita Manatunga (biostatistics and bioinformatics) has been named as the inaugural Donna J. Brogan Professor in Biostatistics. This endowed professorship recognizes Manatunga’s excellence in teaching and research and honors the legacy of Donna Jean Brogan, PhD, emerita professor.
Guido Silvestri has been appointed chair of the Department of Pathology and Laboratory Medicine. Silvestri is a Georgia Research Alliance Eminent Scholar in Comparative Pathology and he serves as director of the Division of Microbiology & Immunology at the Yerkes National Primate Research Center. | |
| |
|

